Preventing Pressure Soars From A Bed
Pressure sores and ulcers happen very frequently from beds. This happens when you do not move from the same position over a long period of time.
How do you help to prevent pressures sores from a bed? Follow these guide lines to help reduce pressure ulcers from happening.
- Use a mattress that is made from foam or that is filled with gel or even air
- Place a soft pillow between body parts so they can help with skin irritation
- If you need to lay on your side it is best to use a pillow that sits between your ankles or knees to help reduce irritation
- If you lay on your back place a pillow under your heels
- Under your calves so it helps to lift your heels
- Under shoulders
Daily Skin Care To Prevent Pressure Sores
Ways to prevent pressure injuries include:
- Checking the skin at least daily for redness or signs of discolouration.
- Keeping the skin at the right moisture level, as damage is more likely to occur if skin is either too dry or too moist.
- Using moisturising products to keep skin supple and prevent dryness.
- Never massaging bony areas because the skin is too delicate.
What Are The Long
If the wound becomes infected, the infection can spread to other parts of the body. Several conditions that may occur if an infection spreads include:
- Cellulitis: An infection of the skin.
- Osteomyelitis: An infection of the bone.
- Bacteremia: An infection of the blood.
- Meningitis: An infection of the brain and spinal cord.
- Endocarditis: An infection of the heart.
Read Also: How Do You Cure Ulcerative Colitis
How To Help Wheelchair Patients Prevent Pressure Ulcers
Anyone that spends a lot of time sitting in a wheelchair is at risk for developing pressure ulcers, often referred to as decubitus ulcers. There are a number of things you and your caregiver can do to prevent the formation of these debilitating sores caused by wheelchairs. This includes hiring a non-emergency medical transportation service that understands the proper techniques for transporting patients in and out of their wheelchair.
Pressure ulcers vary in appearance and severity, starting off as red, irritated skin to full thickness and tissue loss with exposed bone, muscles and tendons. These lesions are often referred to as decubitus ulcers because pressure is only one of many causes.
These lesions can be debilitating and put someone on bed rest for weeks or even months, not to mention the skin may never heal quite right. The older a patient is, the less likely for wounds to heal properly.
Pressure ulcers develop when your skin and soft tissues are pushed against a hard surface for prolonged periods of time. This consistent pressure reduces blood supply to the area, allowing a pressure ulcer to form.
You are at a greater risk for developing pressure ulcers if:
-You spend the majority of your day in a wheelchair or in bed.
-You spend prolonged periods of time in the same position.
-You are either underweight or overweight.
-You are not able to control your bladder or bowels.
-You regularly experience numbness in certain areas of your body.
Caring For A Pressure Sore
Stage I or II sores will often heal if cared for carefully. Stage III and IV sores are harder to treat and may take a long time to heal. Heres how to care for a pressure sore at home.
Relieve the pressure on the area.
- Use special pillows, foam cushions, booties, or mattress pads to reduce the pressure. Some pads are water- or air-filled to help support and cushion the area. What type of cushion you use depends on your wound and whether you are in bed or in a wheelchair. Talk with your health care provider about what choices would be best for you, including what shapes and types of material.
- Change positions often. If you are in a wheelchair, try to change your position every 15 minutes. If you are in bed, you should be moved about every 2 hours.
Care for the sore as directed by your provider. Keep the wound clean to prevent infection. Clean the sore every time you change a dressing.
Avoid further injury or friction.
- Powder your sheets lightly so your skin doesnt rub on them in bed.
- Avoid slipping or sliding as you move positions. Try to avoid positions that put pressure on your sore.
- Care for healthy skin by keeping it clean and moisturized.
- Check your skin for pressure sores every day. Ask your caregiver or someone you trust to check areas you cant see.
- If the pressure sore changes or a new one forms, tell your provider.
Take care of your health.
You May Like: Can I Take Tylenol For Stomach Ulcer Pain
Check The Skin For Signs Of Developing Pressure Sores Often
The skin should be checked frequently for the signs of developing pressure sores. A pressure sore may develop in less than a few hours.
For example, have you ever experienced increased soreness and redness on your buttocks while driving for more than an hour or two? If so, you developed a Stage I pressure sore, but your ability to move allowed you to recognize the pain and adjust your position to prevent it from progressing.
For some seniors, you must be the one to check and recognize the signs of a pressure sores development when performing perineal care, providing showers or performing other assessments of skin integrity. All such checks should be documented as well.
You May Like: Different Types Of Ulcerative Colitis
Causes Of Pressure Ulcers
Pressure ulcers are caused by sustained pressure being placed on a particular part of the body.
This pressure interrupts the blood supply to the affected area of skin. Blood contains oxygen and other nutrients that are needed to help keep tissue healthy. Without a constant blood supply, tissue is damaged and will eventually die.
The lack of blood supply also means that the skin no longer receives infection-fighting white blood cells. Once an ulcer has developed, it can become infected by bacteria.
People with normal mobility do not develop pressure ulcers, as their body automatically makes hundreds of regular movements that prevent pressure building up on any part of their body.
For example, you may think that you are lying still when asleep, but you may shift position up to 20 times a night.
Pressure ulcers can be caused by:
- pressure from a hard surface such as a bed or wheelchair
- pressure that is placed on the skin through involuntary muscle movements such as muscle spasms
- moisture which can break down the outer layer of the skin
The time it takes for a pressure ulcer to form will depend on:
- the amount of pressure
- how vulnerable a person’s skin is to damage
Grade 3 or 4 pressure ulcers can develop quickly. For example, in susceptible people, a full-thickness pressure ulcer can sometimes develop in just 1 or 2 hours. However, in some cases, the damage will only become apparent a few days after the injury has occurred.
Recommended Reading: Treating Leg Ulcers With Sugar
How Can Pressure Injuries Be Prevented
The development of pressure injuries can be prevented through careful observation of the skin and frequent repositioning in those who canât turn themselves. Tips to prevent pressure injuries include:
- Keeping the skin clean and clear of bodily fluids.
- Moving and repositioning the body frequently to avoid constant pressure on bony parts of the body.
- Using foam wedges and pillows to help relieve pressure on bony parts of the body when turned in bed.
- Maintaining a healthy diet to avoid malnutrition and to assist in wound healing.
Express Comfort Contoured Gel Foam Wheelchair Cushion
The Express Comfort Contoured Gel Foam Wheelchair Cushion by the Comfort Company offers a cooling sensation, which not only improves someoneâs comfort but it allows the skin to breathe better while seated. The gel is one of the most sought-after materials for pressure relief cushions, since people find them to be optimally durable and accommodating.
Also Check: Ulcerative Colitis And Lung Disease
Don’t Miss: How To Treat Pressure Ulcers On Buttocks
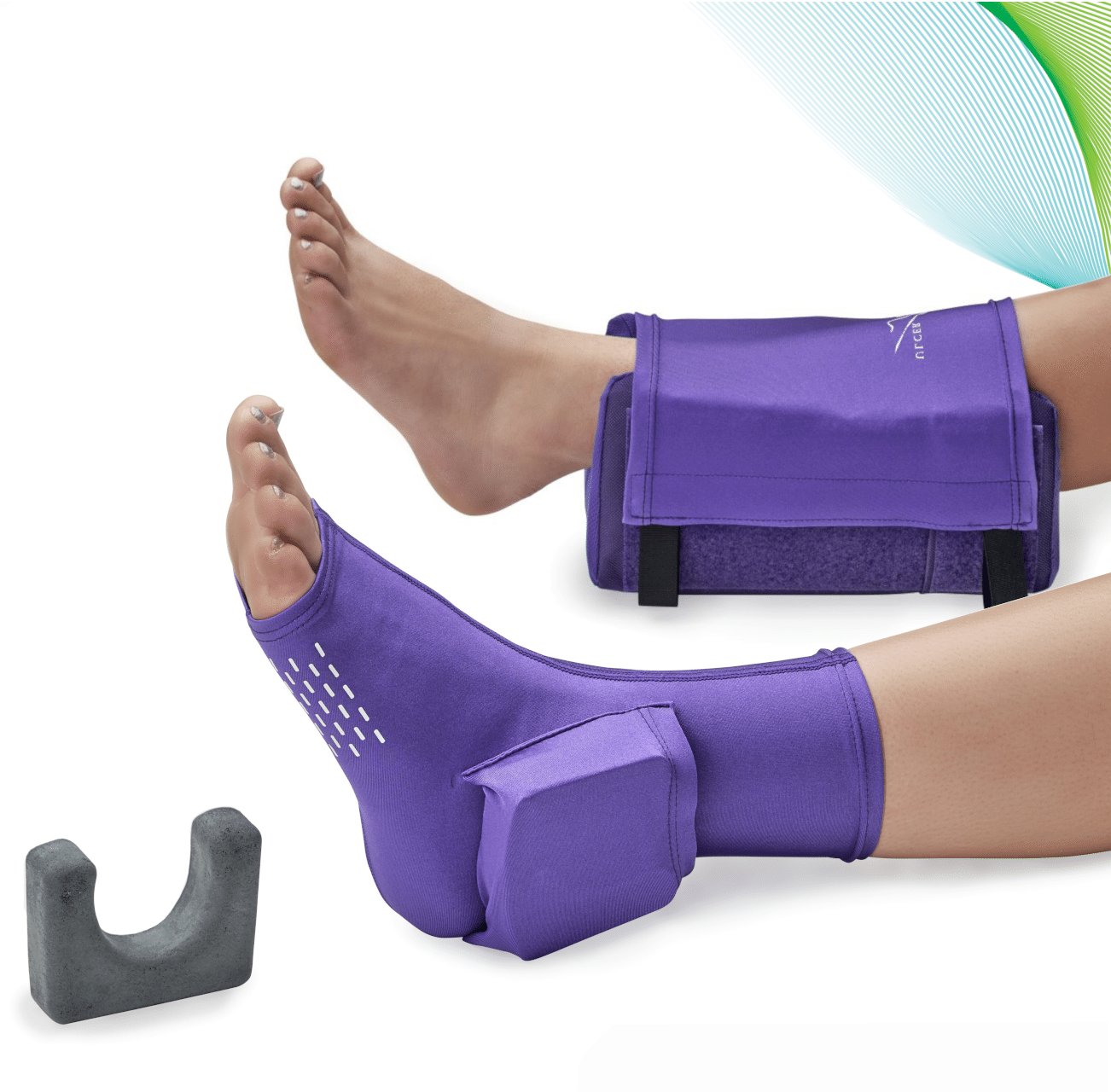
Prevention Of Heel Pressure Injuries
The geometry, anatomy, and perfusion of the heel create challenges in preventing HPIs. International guidelines suggest that to redistribute pressure from the heel, the heel should be floated from the bed. Suspending or floating the heels clear off the support surface by elevating the lower leg or calf is demonstrated to be an effective strategy to relieve pressure, shear, and friction forces, thereby reducing the risk of HPIs. Unfortunately, floating the heel on pillows does not always work if the patient moves about in bed or the pillow collapses from the weight of the leg. In addition, floating the heels will always result in greater weight bearing in other anatomical areas and may shift the risk for injury to elsewhere in the body. When determining which mechanism to use to offload the heel, consider the following issues: How long will the legs be immobile, and how mobile is the patient? Is the patient agitated and moving a lot? Is there poor arterial flow? Are there sensory limitations such as paraplegia or neuropathy? Is the patient is ambulatory? Does the patient slide down in the bed, or do they need a bed extender?
Considerations in Elevating the Heels2
Get Rid Of Your Heel Pain For Good
Whatever your reasons for seeking relief from heel pain and pressure in bed be they comfort and relaxation or a more serious risk of pressure sores we’re sure to have the heel pressure relief solution for you. Since the heels are a particular risk area for pressure ulcers, it may be wise to tackle your pressure problems in yourself or your loved ones before they begin. Pressure sores can be very difficult to heal once they’ve occurred, so tackling the problem when it’s simply a small amount of discomfort is always wise.
Want to take a look at our entire range of products for heel pressure, ranging from the simple to the more elaborate? Take a look at our Heel Pressure Relief category, all available with free UK delivery on all orders!
Do you have any questions about these products, or one of our other pressure relief options? Let us know in the comments, or find us on and !
All major credit and debit cards accepted securely online.We are a trusted ISO 9001:2015 certified company.
020 7720 2266
Our lines are staffed from 9.00am to 5.00pm, Monday to Friday. Health and Care, Unit 6, Union Court, Union Road, London, SW4 6JP.
Also Check: Foods That Heal Ulcers And Gastritis
Can Bedsores Be Prevented
Bedsores can be prevented by inspecting the skin for areas of redness every day with particular attention to bony areas. Other methods of preventing bedsores and preventing existing sores from getting worse include:
- Turning and repositioning every 2 hours
- Sitting upright and straight in a wheelchair, changing position every 15 minutes
- Providing soft padding in wheelchairs and beds to reduce pressure
- Providing good skin care by keeping the skin clean and dry
- Providing good nutrition because without enough calories, vitamins, minerals, fluids, and protein, bed sores cant heal, no matter how well you care for the sore
Description Of The Condition
Pressure ulcers are defined as “a localized injury to the skin and/or underlying tissue usually over a bony prominence, as a result of pressure, or pressure in combination with shear” . Pressure ulcer classification systems provide a method by which the depth and severity of the injury can be described and documented . Pressure ulcers have traditionally been categorised according to severity, from a category I pressure ulcer of intact skin) up to category IV . However, recently two additional categories have been defined ‘unstageable/unclassified’ and ‘suspected deep tissue injury’ . As pressure ulcers are categorised according to depth of the wound, these categories are used when the depth of the wound is unknown. The ‘unstageable’ category describes wounds in which slough or necrosis obscures the wound bed. ‘Suspected deep tissue injury’ describes wounds in which it is suspected that there is deeper damage, such as when bruising or a blood blister is present. Although these additional categories were initially described for use in the USA, they have started to be used and investigated worldwide .
Why is the heel such a high risk area?
Recommended Reading: Colon Cleanse For Ulcerative Colitis
What Are The Risk Factors For Pressure Ulcers:
People with fragile skin are at additional risk, as are people whose nutrition is poor. Diabetes is also a significant risk factor for pressure sores on the feet.
One of the reasons pressure sores are so common among the disabled is that many such people have impaired sensation of pressure and touch due to spinal cord injuries. Because of this, they may not be alerted by pain or discomfort to the need to change position.
People who are bedridden for extended periods may lose a great deal of weight, which reduces the cushioning around their bones, making them more susceptible to pressure sores.
Treatment Of Pressure Ulcers On The Buttocks
Pressure ulcers are a complex health problem whether they are on the buttocks or another area of the body. They can arise as a result many interrelated factors and they can be painful, debilitating and life threatening. Care and treatment of pressure ulcers may be provided by a multidisciplinary team made up of different disciplines of healthcare professionals.
This MDT may include:
- a dietician
- experienced medical and surgical experts
The specific treatment of a pressure ulcer can depend on the stage a pressure ulcer has reached.
Read Also: Ulcerative Colitis And Mental Health
How To Prevent Pressure Sores
Pressure sores are also known as pressure ulcers, or bedsores can happen when your skin press against a surface that is hard for prolonged periods of time. This can happen when someone spends too long sitting in a chair, wheelchair, or bed. The pressure of sitting on a hard surface for too long can slow the blood supply within that area causing the skin or soft tissue to become damaged or even die from an infection. When this occurs a pressure sore or ulcer can form. Lets learn some basic skills on how to prevent pressure sores and know what to look for if you believe you may have one.
For those that fall into the following areas you could be at risk:
- Spend a significant time sitting in a chair
- Spend a significant time in a wheelchair or other mobility device
- Spend a lot of time in a bed without moving much
- Are underweight or overweight
- Spine
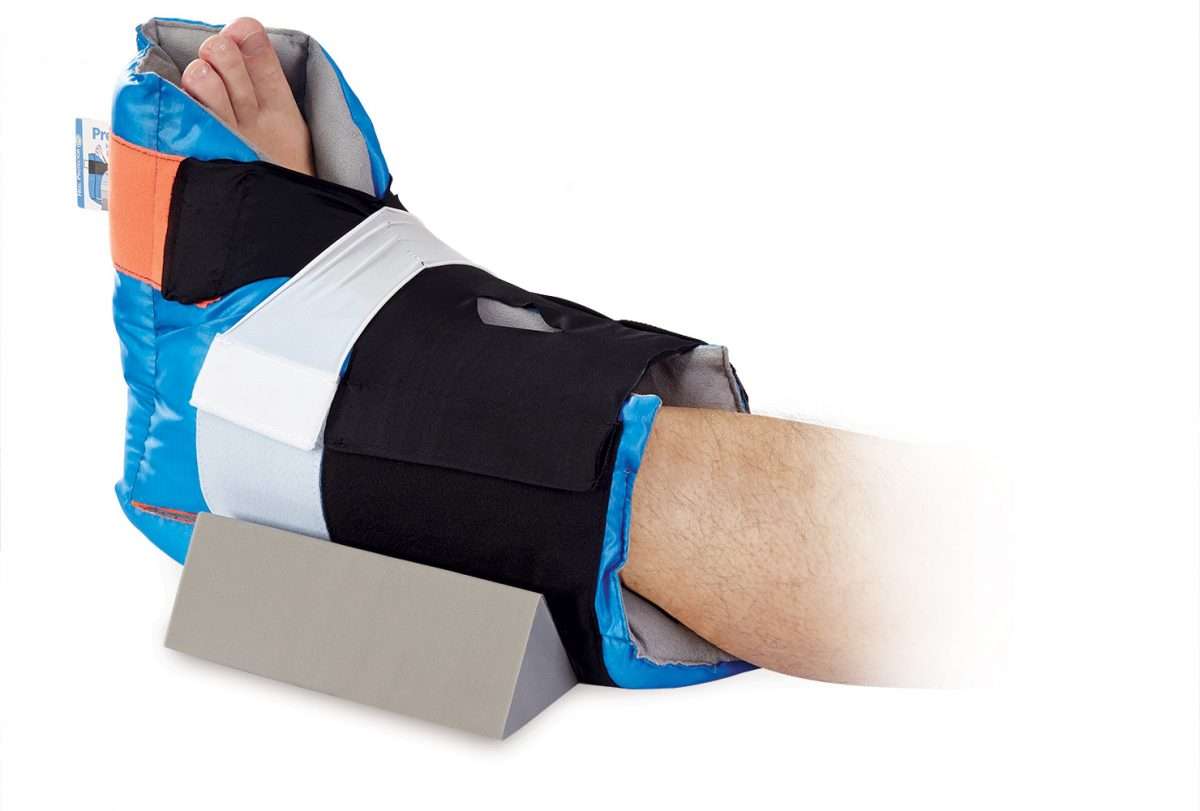
Systam Memory Foam Pressure Relief Heel Boot
For patients at particularly high risk of pressure sores, or for those already suffering from ulcers, more serious measures may be necessary. Suited to post-surgical recovery or patients in intensive care, the Systam Memory Foam Pressure Relief Heel Boot provides powerful pressure relief with moulded memory foam that is shaped to prevent equinus distortion and rotation a particularly heinous risk factor for pressure sores.
The zone at the base of the heel is completely cut away, enabling the heel to be entirely suspended for complete relief of pressure. A valley on the boot prevents excess pressure on the achilles tendon, making the boot a complete pressure relief solution for the lower legs.
Key Features: Moulded with foam to completely suspend the heel, prevents rotation for powerful and all-encompassing pressure relief.
You May Like: Best Diet For Gerd And Ulcers
Immobility Shear And Friction
Patients who spend significant periods of time in a supine position, for example those on extended bedrest, may find that their feet tend to abduct . This rotation causes pressure to pass through the lateral aspect of the heel to the calcaneus, where the fat pad is thin and irregularly shaped . Patients who have undergone surgery are at increased risk of heel pressure ulcers because analgesia and anaesthesia reduce their pain responses to pressure and because they are immobilised for prolonged periods . Orthopaedic and vascular surgical interventions may require postoperative immobilisation of the lower limb.
Shear and friction are common extrinsic factors increasing the risk of heel pressure ulcers. Shear occurs when the bones and the skin move in opposite directions for example during suboptimal repositioning where the patient is pulled along the bed and is a common issue in patients with suboptimal mobility . Shear affecting the heels can occur if the patient slides downwards due to inadequate positioning in a chair or bed, or if the patient uses their heels as a pivot point when repositioning themselves. Friction can be described as the mechanical force exerted when a patient is moved across a coarse surface such as bed sheets, which prevents the skin from sliding along smoothly . Friction to the heel can be caused by a suboptimal moving and handling technique or by frequent foot movements, for example in patients experiencing tremors or agitation.
Provide Protection Against The Heels Unique Vulnerability To Pressure Ulcers/injuries
The heel is uniquely vulnerable as a pressure ulcer site the second most common site after the sacrum according to a recent study of almost 450,000 patients .
The heel is especially sensitive for a number of reasons :
- Low blood flow to heel area
- Less soft tissue padding over the bony prominence
- Shear forces from patient sliding in bed
Read Also: What Medicine Is Best For Stomach Ulcers
Identifying The Different Stages Of Heel Pressure Ulcers
- Stage 1 The area will appear red and feel warm to the touch. This is usually accompanied by a burning, itching, and/or painful sensation.
- Stage 2 The damaged area has partial-thickness skin loss and may appear as a shallow wound or as an intact or ruptured blister. There will be considerable pain and the skin surrounding the area may also be discolored.
- Stage 3 Damage has reached the deep tissue below the surface causing the wound to have a crater-like appearance and there will be a loss of sensation to the area.
- Stage 4 The area is severely damaged and the wound has deepened. Muscles, tendons, bones, or joints may be visible in the wound at this stage.
It is of utmost importance to identify and treat pressure wounds on heels at the earliest stage. If you notice a red area, apply pressure with your fingers. If the redness remains after you release the pressure, change positions to alleviate pressure from the area and monitor closely. If there is no improvement, or the condition worsens, contact your doctor in 24 to 48 hours.