What Is A Kennedy Ulcer Symptoms And Diagnosis
What is a Kennedy ulcer? What are the symptoms? And how do you treat it? Lets find out. In this article, well explain what the symptoms of this ulcer are. Also, well explore how to diagnose a Kennedy ulcer. Here are the most common symptoms of a Kennedy ulcer. If you suspect you may have one, its important to seek medical attention as soon as possible. There is no cure for a Kennedy ulcer.
Bed Sores In End Of Life
At end of life there will be many rapid changes and deterioration in an individual and many of these will come to the skin in the final stages of life. One of these skin conditions that can come quickly and in a devastating manner are painful and mostly untreatable Kennedy ulcers.
Kennedy ulcers are not fully understood and the medical community has not come to an absolute consensus on how to define it, treat it, or even categorize it.
What is known is that this kind of ulcer is a sign of tissue death that can come on rapidly and has little to no treatment in the traditional sense of the word.
Rather, it is believed that a better way to understand the Kennedy ulcer is to see it as an end of life change in the skin that may not be treated with traditional preventative methods used on other pressure wounds.
Specifically, the Kennedy ulcer, along with a few other skin conditions are listed as a SCALE, or a skin change at lifes end which has its own needs and norms in nursing care and is a phenomenon that is still in need of extensive further research.
Because of the many unknowns with Kennedy ulcers, the most important aspect of them is to ensure that the individual who is suffering from them has the care and attention that they need to ensure their pain is managed.
Medical Malpractice Nursing Home Abuse Lawyer Near You In Baltimore Maryland & Beyond
I can help you anywhere in Maryland, including Allegany County, Anne Arundel County, Baltimore City, Baltimore County, Carroll County, Calvert County, Caroline County, Cecil County, Charles County, Dorchester County, Frederick County, Garrett County, Harford County, Howard County, Kent County, Montgomery County, Prince Georges County, Queen Annes County, Somerset County, St. Marys County, Talbot County, Washington County, Wicomico County, and Worcester County.
I have helped clients in over a dozen jurisdictions, including California, Delaware, District of Columbia, Georgia, Illinois, Iowa, Massachusetts, Maryland, Mississippi, New Jersey, New Mexico, New York, North Carolina, Pennsylvania, South Carolina, Washington, and Virginia.
I help injured victims nationwide in all 50 states on a case-by-case basis via Pro Hac Vice.
Don’t Miss: Best Fruits For Ulcerative Colitis
Use Of A Kennedy Ulcer Diagnosis To Conceal A Bedsore
Occasionally, our lawyers will investigate a case where a facility diagnoses a patients wound as a Kennedy terminal ulcer, but the wound has all the signs of being a garden variety bed sore. This may be done as a way to cover up neglect of the patient, since Kennedy ulcers just happen while bed sores really should not occur.
If you think your family member received a misdiagnosis of a Kennedy ulcer, compare the above factors and see which kind of wound closer fits the description of your family members ulcer.
Cms Recognizes The Kennedy Terminal Ulcer In Long
by Jeffrey M Levine | Jul 10, 2013
The Kennedy Terminal Ulcer has been around for over two decades, and continues to play a large part in discussions as to whether pressure ulcers are avoidable or unavoidable. Until now the Center for Medicare and Medicaid Services has not acknowledged the KTU in its regulatory and reimbursement guidelines for hospitals and nursing homes. In a new transmittal from CMS, the KTU can now be used to avoid reporting a pressure ulcer as a quality measure in Long-Term Care Hospitals . This step goes a long way in legitimizing the concept that certain medical conditions can lead to unavoidable pressure ulcers that are not indicative of inadequate quality of care.
Long-Term Care Hospitals are also known as Long-Term Acute Care Hospitals or transitional care hospitals. These are facilities licensed as acute care hospitals with additional Medicare certification that supports a length of stay more than 25 days. The LTCH is sometimes the only choice for people who have been in an acute-care hospital but are too sick to return home or go to a skilled nursing facility or rehabilitation setting. LTCH patients are medically complex, and because of the heavy burden of co-morbidities one can expect wound care to be a common concern.
These instructions potentially eliminate , new pressure ulcers in persons who are expected to die from quality indicator reporting in Long-Term Acute Care hospitals.
Recommended Reading: Manuka Honey Used For Ulcerative Colitis
Nursing Home Patient Kennedy Terminal Ulcer Lawyers: Chicago Illinois
Nursing home residents face all sorts of risks during their stay at long-term care facilities, but none may present a more sizeable or imminent danger than Kennedy Terminal Ulcers. Referred to colloquially as KTUs, these fast-growing ulcers may spell death for a patient in just a few hours, which is normally the same amount of time they take to form. Often pear-shaped and found in the lower back area of the spine , they can be spotted by their purple color, and this is a sign of sure trouble soon on the horizon.
The Chicago nursing home attorneys at Rosenfeld Injury Lawyers represent patients and families of victims who have suffered because of Kennedy ulcers in Illinois nursing home. While KTU’s are a special case of pressure sores, they nonetheless implicate similar medical issues. However, on substantial legal and medical points, they also differ. The sections that expound upon these matters. If you have more questions or concerns, call us anytime and with no obligation at 424-5757.
Causes Of Kennedy Terminal Ulcer
The exact cause of Kennedy terminal ulcers is unknown. â
Some experts say that it may be due to your organs shutting down. Your skin is your bodyâs largest organ. It’s about 10% to 15% of your total body weight. It uses about 25% to 33% of the amount of blood that your heart pumps in 1 minute, or your cardiac output.
Like other organ systems, it can fail, especially as you age.
Your skin can reflect signs of illnesses. Some illnesses that affect your whole body can cause characteristic effects on your skin. For example, if you have liver disease, you’re likely to have swollen blood vessels and reddish palms .â
While the cause hasnât been determined, most people develop Kennedy terminal ulcers in their final weeks of life. Further studies are needed to better understand these ulcers.
Recommended Reading: Ulcerative Colitis Pain After Eating
The Presence Of Ulcers In Long
Ulcers and sores are not rare occurrences in long-term care. However, this does not mean wounds are an acceptable outcome of a long term care residency.
One of the most common varieties is the pressure ulcer, which is also sometimes referred to as a pressure sore, pressure injury or a bedsore. Any resident of a nursing home who develops a bed sore should be attended to immediately, and the family should investigate legal action against the nursing home for negligence. Bedsores are not an acceptable part of an aging loved ones health situation.
Conversely, a sore that at first glance appears to be a bedsore could turn out to be a Kennedy terminal ulcer. Kennedy ulcers are treated differently and do not arise from the same causes that create bed sores. Still, Kennedy ulcers are oftentimes misdiagnosed as pressure ulcers. Similarly, pressure ulcers are commonly misdiagnosed as Kennedy terminal ulcers if the patient is dying.
It is vital that you understand the difference between the two so that you can advocate for proper care for your loved one or family member.
How Is A Kennedy Ulcer Managed
As mentioned, a Kennedy ulcer isnt typically treated. However, because its a sign of approaching death, sometimes management involves:
- Ensure patient comfort with pillows under ulcers
- Manage any pain in patient
- Emotional support for the family during the patients end of life
Other than the focus on patient comfort, nurses may also notify the family of approaching death.
Also Check: Besivance Dosage For Corneal Ulcer
Kennedy Terminal Ulcer Treatment
As their name suggests, Kennedy ulcers normally signal that a patient has entered a final phase of their life. It is probable that comorbidities in addition to KTUs are critically threatening his or her life. At this point, medical teams normally switch to preserving a person’s quality of life with palliative care.
This can be done through a number of options including surgical methods, medication, repositioning, and other means of medical and daily assistance. The exact course will be chosen by a doctor in consultation with the nursing home resident and his or her family.
Kennedy Terminal Ulcer Symptoms
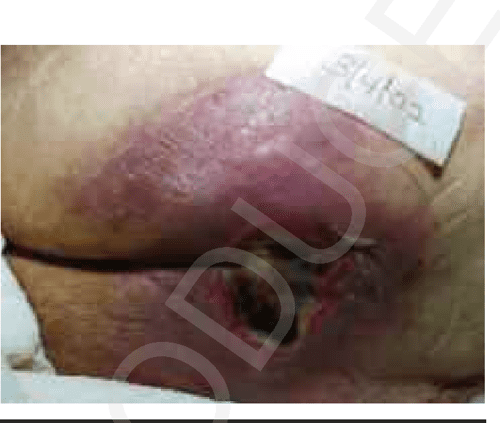
Differentiating between Kennedy ulcers and other types of bruises, sores, or lesions can be difficult at times. Plus, their quick emergence makes identification hard in the first place. Yet, Kennedy ulcers do have some distinctive signs and symptoms to alert you to their presence such as the following:
- Kennedy ulcers normally pop up on a person’s sacrum, the lower triangular spot on the back/pelvis.
- Kennedy ulcers normally are pear-shaped initially though that might morph into a difference shape later.
- Kennedy ulcers normally have similar colors to other bruised parts of the body: blue or purple and black as it gets much worse.
- Kennedy ulcers normally develop very quickly unlike bed sores.
Recommended Reading: Types Of Steroids For Ulcerative Colitis
Kennedy Terminal Ulcers From A Nursing Expert Witness Perspective
The Kennedy Terminal Ulcer is an area of skin breakdown that develops when a person is dying and/or in multi-organ failure. The term KTU was named after Karen Lou Kennedy, a Family Nurse Practitioner, who in 1983 first started the process in differentiating this type of skin breakdown from standard pressure ulcers/injuries. In 1989 the National Pressure Ulcer Advisory Panel formally recognized KTUs, by defining them as an unavoidable skin breakdown related to the dying process having certain identifying characteristics that differentiate them from traditional pressure ulcers/injuries. The Center for Medicare and Medicaid Services has also adopted the definition and differentiation of kennedy terminal ulcers from standard pressure ulcers/injuries. In order to differentiate a KTU from a standard pressure ulcer/injury, it is essential to immediately identify the characteristics:
- Usually located on a sacrococcygeal area, however, can also appear on the heel, elbow, calf, or arm
- Appear to be shaped like a pear, butterfly, or horseshoe
- Red, yellow, black, blue and/or purple in color
- Presence of irregular borders
- There is a sudden onset.
Immediate assessment and documentation upon presentation by the nurse or staff is vital to ensure appropriate diagnosis and interventions are implemented. Accurate diagnosis of a KTU is dependent on the review of the patients medical history to determine if death is imminent and the clinical presentation of the skin breakdown.
Why Is It Called Kennedys Disease

The disorder is named after William R. Kennedy, MD, who reported it in an abstract in 1966 and a complete report in 1968. Dr. Kennedy was a neurologist at Johns Hopkins Hospital in Baltimore.
It affects the brain’s nerve cells, which control movement. As these cells die, it becomes difficult to move muscles, especially those used for walking. People with Kennedy’s disease eventually become wheelchair users. There is no cure for this disease.
The incidence of Kennedy’s disease is unknown. It is found almost exclusively in men however, women can get it too. Usually people develop Kennedy’s disease between the ages of 45 and 75. However, children have been known to get it as well as older people.
The diagnosis of Kennedy’s disease can be difficult because its symptoms are similar to those of other diseases and conditions that affect the brain such as Alzheimer’s disease, Parkinson’s disease, and multiple sclerosis. A biopsy of the spinal cord’s nerves or brain tissue is needed to confirm the diagnosis.
There is no treatment for Kennedy’s disease. The goal of care is to make patients as comfortable as possible by providing support systems for their arms and legs, as well as cognitive and psychological counseling.
About Article Author
You May Like: What Is The Recommended Diet For Horses With Ulcers
How Are They Treated
Kennedy ulcers usually signal the start of the dying process, and theres no way to get rid of them. Instead, treatment focuses on making the person as comfortable and pain-free as possible. Depending on where the ulcer is, this might involve placing a soft cushion under the affected area.
If a loved one has a Kennedy ulcer, this may be a good time to invite other loved ones in to say goodbye. If youre not there, their care team of doctors and nurses may call on you to be by your loved ones side in their final moments.
Are Kennedy Ulcers Preventable
While bedsores are entirely preventable with regular shifting of an individuals body weight, Kennedy terminal ulcers are a natural part of the process of passing away. Regular, vigilant care must still be taken, since Kennedy ulcers can be hastened by extended pressure on the skin. However, even the best care cannot completely stop the effects of the bodys internal systems shutting down.
Also Check: Symptoms Of Bleeding Ulcer In Esophagus
What Are The Symptoms
It can be hard to distinguish between a pressure sore or bruise and a Kennedy ulcer at first glance. However, Kennedy ulcers have a few unique characteristics that you can look for:
- Location. Kennedy ulcers typically develop on the sacrum. The sacrum is a triangle-shaped area of the lower back where the spine and pelvis meet. This area is also sometimes called the tail bone.
- Shape. Kennedy ulcers often start as a pear- or butterfly-shaped bruise. The initial spot may grow rapidly. You may observe various shapes and sizes as the ulcer spreads.
- Color. Kennedy ulcers can have a range of colors, similar to a bruise. You may see shades of red, yellow, black, purple, and blue. In its later stages, a Kennedy ulcer starts to become more black and swollen. This is a sign of tissue death.
- Onset. Unlike pressure sores, which can take weeks to develop,Kennedy ulcers pop up suddenly. It may look like a bruise at the start of the day and an ulcer by the end of the day.
- Borders. The edges of a Kennedy ulcer are often irregular, and the shape is rarely symmetrical. Bruises, however, may be more uniform in size and shape.
Treatment Of Kennedy Ulcers
Treatment options for a Kennedy ulcer are limited. When a person has entered into the Kennedy ulcer later stages, it can often mean that this is an individuals final stages of life.
In many people with a terminal Kennedy ulcer, there is an unavoidable skin breakdown which is happening as a part of the dying process and cannot be treated.
These final stages, also known as the unstageable periods, are usually accompanied with full thickness tissue loss and the presence of a layer of slough over the ulcer which can be yellow, brown or green in color.
When this happens, there is no treatment to actually address the ulcer anymore, and the plan of care shifts to ensuring comfort, respect and dignity in the final hours, days or weeks of life that a person has.
Don’t Miss: Mouth Ulcer On Gum Causes
Pressure Wounds Do Not Precede Death
On the other hand, nursing homes often try to hide their malpractice by labeling a regular pressure wound as a Kennedy Ulcer. Thats the nursing home trying to lie and say, this person was going to die anyway.
Do not fall for this. Have a lawyer look at the medical records, the timeline of the ulcer, its progression, its coloration, size, and other features, to help you figure out if the nursing home is involved in a cover up.
A Butterfly That May Herald End Of Life
Barbara Zeiger
The Ostomy Wound Management website is experiencing an uptick in searches for information regarding the Kennedy Terminal Ulcer . This pressure ulcer exhibits unique properties: sudden occurrence and rapid progression usually located in the sacral/coccygeal area1 most often butterfly-shaped, but also pear-, horseshoe-, or sometimes irregular-shaped and with red/yellow/black highlights that may look similar to an abrasion or blister.1 Its fragile blister roof may decline quickly from being intact to becoming an open wound merely as the result of gentle cleansing the periwound and underlying skin may be soft and loose. Despite initially demonstrating the characteristics of early deep tissue injury, the ulcer may darken before demarcating, with a metamorphosis to a Stage II, Stage III, or Stage IVulcer occurring from within 24 hours to up to 5 days.3,4
Skin Failure
According to the 2008 American Medical Directors Association guidelines,12 the section on pressure ulcers includes the KTU as an unavoidable ulcer, and the KTU is included in the National Pressure Ulcer Advisory Panels13 updated pressure ulcer staging system. Literature addressing the provision of evidence-based palliative or end-of-life care includes information on the KTU.14
The Clinicians Role
Assess the skin, paying particular attention to areas such as bony prominences most at risk for compromise
Address comorbidities
References:
Read Also: Can Acid Reflux Cause Ulcers
Kennedy Ulcer : 30 Syndrome
While most Kennedy ulcers tend to develop out of the blue and without warning begin to rapidly progress, some are even faster and more devastating.
A phenomenon known as the 3:30 syndrome is a Kennedy ulcer that can present initially as a speck of dirt and then within a few hours can spread and go from the early stages of a bruise to a dark black patch of skin that gets increasingly larger in a short burst of time.
A 3:30 syndrome Kennedy ulcer is often seen as a bed sore at end of life because a person with 3:30 syndrome Kennedy ulcers generally only has a life expectancy of 8-24 hours.