What To Do If You Or A Loved One Has A Decubitus Ulcer
The first thing to do if you find out that you or someone you love has developed a bedsore is to demand immediate treatment. Skincare specialists and wound specialists may help you in this situation. Do everything you can to increase nutrition intake and repositioning practices of the nurses and health care staff responsible for the patients diet and daily skin care.
If the pressure sore appears in the hospital, nursing home or assisted living facility, you may want to seek legal help in addition to medical treatment. In most cases, pressure sores are easy to prevent if nurses or other health care providers take the time necessary to assess the patients risk and provide proper preventive measures. If they failed to do so, these medical providers may be liable to pay for the pain, suffering and bodily injury they have caused.
Medical malpractice cases are actually quite common. In fact, over 200,000 people die from medical malpractice incidents every year in the United States. These cases often have very high returns due to the extensive medical treatment costs and the severe consequences of inappropriate treatment.
How Do Pressure Sores Begin
Pressure sores develop for many reasons, so hospitals should have strategies in place to screen for risks among all of their patients. However, there are certain environments that lend themselves particularly to pressure injury development, including moisture, shear, advanced age, limited mobility and lack of access to monitoring technology. Its important to be vigilant with proactive screening for bedsore development, especially with high-risk patients.
Here are the early warning signs of a pressure sore:
- Discoloration or dark skin, whether redder, bluer or more purple than usual
- An area of skin feeling warmer to the touch than surrounding skin
- Skin that feels firmer in one spot than usual
- Itchy, painful skin
- When the skin is pressed down on, it doesnt appear lighter
- Swelling on the skin
Recommended Reading: What Does An Ulcer Look Like
Severity Of Pressure Ulcers
Healthcare professionals use several grading systems to describe the severity of pressure ulcers most common is the EPUAP grading system. Pressure sores are categorised into four stages corresponding to the depth of damage. It must however be emphasised that when an eschar is present, accurate staging is not possible.
Don’t Miss: How Can You Get Ulcers In Your Stomach
Signs And Symptoms Of Pressure Ulcer
The general clinical manifestations of pressure ulcers include:
- Unusual skin color or texture discrepancies
- Erythema or redness
- Edema or swelling in the affected area or limb
- Discharges foul in odor, can be fluid or pus-filled
- Warm or cold to touch An area of the affected region that feels different to touch than surrounding areas
- Tenderness and pain on site
How Are Bedsores Caused
Bed sores, also called pressure ulcers or decubitus ulcers, are injuries to the skin and underling tissue resulting from pressure on skin. Bed sores often occur when nursing home residents are immobile or bedridden and develop on parts of the body that make the most contact with surfaces- tailbone, ankles, heels, and hips.
Bed sores develop in four stages. In stage one, the skin begins to turn red and may feel warm. It may be painful to the touch. In stage two, the wound opens as the skin breaks down. In stage three, the wound area becomes deeper as more tissue begins to die. In stage four, there is large scale tissue loss.
When bed sores progress to the later stages, they can lead to other complications that are fatal for nursing home residents. Three of the more common deadly problems arising from bed sores are osteomyelitis, , and gangrene.
Osteomyelitis: This condition is an infection of the bone. The infection starts at the affected tissue, moves into the bloodstream, and then travels to the bone. Often the infection can begin in the bone at stage 4.
Sepsis: Sepsis is a condition in which bacteria from the bed sore enters the bloodstream an infects other parts of the body. Sepsis may lead to organ failure and death if not treated quickly.
Gangrene: This is a condition where the bodys tissue dies due to loss of blood supply. In residents with bedsores, the loss of blood supply is the result of infection from the wound area.
Read Also: How To Calm An Ulcer
Are We Ready For This Change
Because pressure ulcer care is complex, efforts to improve pressure ulcer prevention require a system approach that will involve organizational change. Bringing about organizational change of any type is difficult. It is even more difficult when it involves multiple, simultaneous modifications to workflow, communication, and decisionmaking as are needed in a pressure ulcer prevention initiative. Failure to assess your organization’s readiness for the change at multiple levels can lead to unanticipated difficulties in implementation, or even the complete failure of the effort. Each of the questions below will help you and your organization explore readiness and identify action steps to improve it, if necessary.
Who Is Most Likely To Die From Bedsores
Although bedsores can kill persons of all ages and backgrounds, there are certain populations that are more susceptible.
- Advanced Age.People 64 years or older are more likely to suffer from bedsores and death.
- Nursing Home Residents. Recent studies show that over one quarter of all instances of pressure ulcers occur in nursing homes. In fact, in 2004, 11% of all nursing home residents in the country had bedsores. Most nursing home residents have multiple risk factors, including immobility, sensory deficiency, and incontinence.
- Circulatory Problems. Bedsores are more likely to occur when blood flow is already impaired due to a chronic illness associated with circulation.As such, persons with a diagnosis of stroke, hypotension, diabetes of any type, coronary artery disease, and hypoxia are at heightened risk.
- Pulmonary and Renal Problems. Bedsores tend to develop more often when blood cannot be oxygenated, or when red blood cells are prevented from being generated by the body. Therefore, persons with pulmonary disease, end stage renal failure, or severe anemia are at increased risk.
- Malnutrition. Nutrition plays a large part in healing wounds. When a resident has chronic conditions that impair nutrition intake, the likelihood of death increases. Persons with dysphagia, diarrhea, and cancer may be at increased risk of death from bedsores.
Don’t Miss: How To Treat Rodent Ulcers In Cats At Home
How Does Bad Nursing Home Care Cause Bedsores
Every nursing home is required by Federal and state law to take precautions aimed at reducing bedsore occurrences. In fact, the Centers for Medicare and Medicaid Services may cite a nursing home for failing to take the proper precautions. So what are those requirements?
- Comprehensive Assessment. Every resident admitted to a nursing home must be assessed from head to toe for skin impairments. Also, the facility must calculate the residents risk level for developing bedsores.
- Care Plan. Once the assessment is conducted, the data acquired is used to create an action plan. Called a care plan, this document details the ways in which the nursing home should prevent bedsores. For example, a proper turning/repositioning regime or an increase in protein intake at meal time.
- Update Care Plan. Assessment does not stop after the care plan is created. If problems arise afterwards, then the nursing home is obligated to update the care plan with new ideas and interventions.
Bad care means that the nursing home fails to complete one of the three steps above. Essentially, the resident that comes into the nursing home with no bedsores should leave the nursing home with no bedsores.
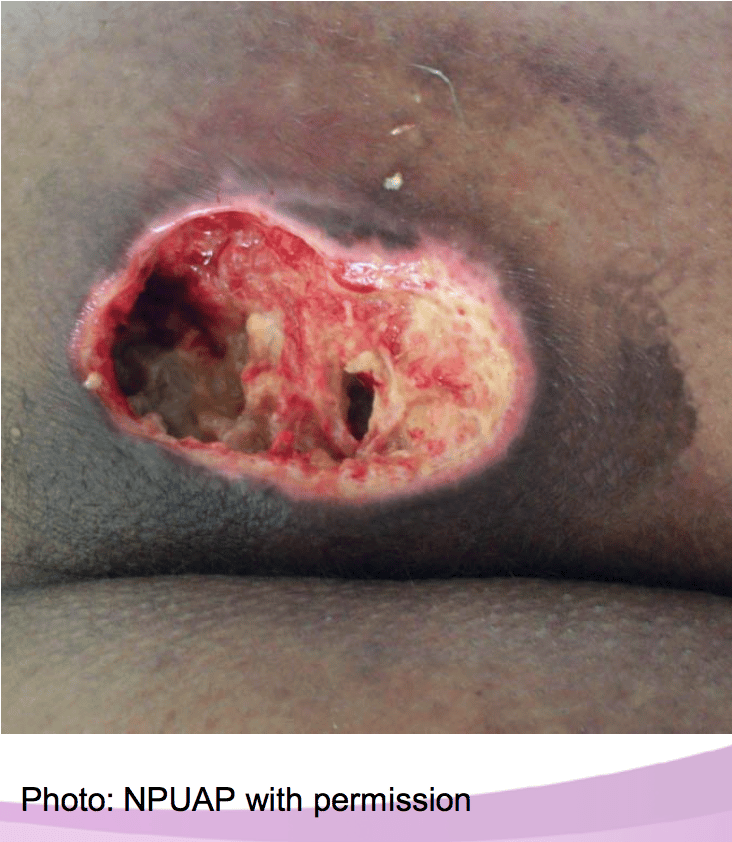
Stage 4 Bedsore / Decubitus Ulcer
Stage 4 Bedsore is the last and most serious stage of all bedsores. In a stage 4 bed sore the patient has large-scale destruction of tissue, muscle and skin occurs. Such massive loss of tissue can also include, along with damage to muscle, bone, and even supporting structures such as tendons and joints. Stage 4 bed sores or decubitus ulcers usually require surgery to remove decayed or necrotic tissue. If aggressive treatment of a stage 4 bedsore is not taken, then further necrosis and infection can lead to septacemia, possible needed amputation and even death.
Stage 4 medical treatment include debridement, constant changing of dressing & cleansing for proper wound care, electrical stimulation and surgery. Stage 4 surgery may consist of excising of pressure ulcer, surrounding scar, bursa, soft tissue calcification, and underlying necrotic or infected bone. On deeper stage 4 bedsores and decubitus ulcers a flap surgery is needed to close the wound, fill in the dead space thus enhancing vascularity of the healing wound, and distributing pressure off the bone. All stage 4 bedsore were Stage 3 bedsores at one time, but due to the lack of quality medical and nursing care, the pressure sore continued to get worse and progressed.
Neglect is the Major Cause of a Stage 4 Bedsore
Donât Miss: Is Keto Good For Ulcerative Colitis
Recommended Reading: Why Won T My Mouth Ulcer Heal
Family And Individual Level
Healthcare professionals can have an impact on an individual level by:
- recognising the important role individuals, families and carers have in preventing and managing pressure ulcers
- engaging individuals, carers and families in what to look for and how pressure ulcers can be prevented
- using appropriate literature with visual images to explain how quickly pressure ulcers can develop
- educating the individuals and caregivers about the causes, assessment and management of pressure ulcers
- using appropriate terminology recognising and informing patients that pressure ulcers are another term for bed sores
- encouraging individuals to move independently whenever possible
- directing individuals to appropriate healthcare professionals if they suspect a pressure ulcer is forming or is present
- looking out for skin discolouration or soreness, particularly in areas where bones are close to the skin
- repositioning or turning patients frequently at least every 2 hours for those patients who need help
- using moving and handling aids to help reposition individuals who require assistance moving
- performing regular skin inspections to check areas at risk and document pressure areas at least once a day
- checking that patients with pressure ulcer risk factors are registered with a GP and receive primary health care support to minimise the risks
- providing holistic health assessments for people at risk of developing pressure ulcers
Patient Characteristics At Index Hospitalisation
A total of 9677061 patients were included in the study, of whom 46108 developed a HAPI during the index hospitalisation. Of the 46108 HAPI patients, 7503 were Stage 1, 18901 Stage 2, 3242 Stage 3, 1310 Stage 4, 3358 unstageable, 6754 unspecified and 5040 patients had missing information for stage . Patients with Stage 4 HAPIs had higher percentages of quadriplegia/hemiplegia, shock, sepsis, history of previous pressure ulcer, and malnutrition compared with patients in other HAPI stages. Percentages of patients with any days of ICU stay during the index hospitalisation differed across HAPI stages as well, with the highest in Stage 4 and the lowest in Stage 1 . Average propensity scores were also highest in the Stage 4 HAPI group and lowest in Stage 1 .
| No HAPI |
|---|
Also Check: Foods That Cause Stomach Ulcers
Treatment Of Stage 3 And Stage 4 Pressure Ulcers
The goal of treatment for stage 3 and 4 pressure ulcers, is to properly debrideand dress the wound cavity, create or maintain moisture for optimal healing, and protect the wound from infection. The goal of properly unloading pressure from the area still applies. At these pressure ulcer stages, more emphasis should be placed on proper nutrition and hydration to support wound healing. If the extent of the pressure ulcer or other factors prohibit it from healing properly, surgery may be necessary to close the wound.
The following precautions can help minimize the risk of developing pressure ulcers in at-risk patients and to minimize complications in patients already exhibiting symptoms:
- Patient should be repositioned with consideration to the individualâs level of activity, mobility and ability to independently reposition. Q2 hour turning is the standard in many facilities, but some patients may require more or less frequent repositioning, depending on the previous list.
- Keep the skin clean and dry.
- Avoid massaging bony prominences.
- Provide adequate intake of protein and calories.
- Maintain current levels of activity, mobility and range of motion.
- Use positioning devices to prevent prolonged pressure bony prominences.
- Keep the head of the bed as low as possible to reduce risk of shearing.
- Keep sheets dry and wrinkle free.
Can You Sue A Nursing Home For Bedsore Death

Yes. You can sue a nursing home if a loved one has died as a result of bedsores. In fact, often other entities associated with the nursing home may be sued as well. These entities include management companies, shell corporations, the main office, and others. Further, individuals may be sued as well, like the owners, the administrator, and directors.
Often there are two claims: The Estate of the deceaseds claim for personal injury and the claim by the relatives called wrongful death. The Estate may be entitled to recover damages for pain and suffering, medical bills, funeral expenses, and other related expenses. The wrongful death claim holders may be entitled to recover for the loss of value of the life of the resident.
Don’t Miss: Draw Sheets Are Used To Prevent Pressure Ulcers
Stage 4 Bedsore Prevention
The best way to prevent a stage 4 bedsore is by being proactive.
To prevent stage 4 bedsores, you can:
- Avoid buttons on clothes and wrinkles in bedding
- Avoid doughnut cushions, as they can add pressure to surrounding areas
- Change bedding and clothing on a regular basis
- Check skin daily
- Consider specialty wheelchairs that can be tilted to relieve pressure
- Elevate bed to no more than 30 degrees at the head
- Have the resident perform wheelchair pushups if possible
- Keep skin clean and dry
- Make sure youre repositioning at least once an hour
- Purchase special mattresses or cushions to position the body properly
- Use moisturizing skin care to protect the skin
Remember: Nursing home staff members are trained to prevent stage 4 bedsores. They may be to blame if your loved one developed a stage 4 bedsore while living in a long-term care facility.
You can hold nursing home staff accountable for bedsores. Chat with us now to learn more.
Factors That Influence Sacral Ulcer Management
While wound management is a key part of sacral ulcer management, treating patients holistically is the key to success. Apart from ischemia, other factors that impede normal healing include poor nutrition, infection, edema, persistent moisture, fecal and urinary soiling, and shearing forces. One can look for, prevent, or minimize each of these risk factors. Of course, the patient should be frequently repositioned to avoid further tissue damage and to promote healing.
When selecting a dressing, the wound should be kept moist but not contain excessive amounts of exudate. Wound care professionals should consider the type of ulcer and any comorbid conditions that could complicate treatment . Arterial wounds generally require a moisture-retaining dressing, while wounds that arise from venous insufficiency usually require a dressing that absorbs excess moisture. All surfaces of the wound, including any tunnels, should be packed with the appropriate dressing.
Read Also: How Do Doctors Test For Ulcerative Colitis
Read Also: Does Ulcerative Colitis Cause Fatigue
Whos At Risk Of Stage 4 Bedsores
Anyone with a lower-stage bedsore is at risk of a stage 4 sore. However, some patients may be more prone to this type of injury.
At particularly high risk are those:
- With Limited MobilityMovement is the key to preventing bedsores of any stage. If an older person cannot move on their own, they may sit or lie in the same position for hours. This can cut off blood flow to their skin and cause a bedsore.
- Who Are In Understaffed Nursing HomesNursing home residents with mobility issues must rely on staff members to prevent bedsores. Sadly, some care facilities may fail to prevent bedsores due to issues like understaffing and poor training.
- Who Have Alzheimers or DementiaIf residents with mental impairments develop a bedsore, they might not be able to tell anyone due to their condition. Theyll need to have someone else find it and help them get the proper care. Residents with these conditions may also have trouble sensing pain.
- Other FactorsResidents are at higher risk of bedsores if they have blood flow or circulation problems, diabetes, or poor nutrition or if they wear a cast.
Stages Of Pressure Ulcers And Treatment
Pressure ulcers can progress in four stages based on the level of tissue damage. These stages help doctors determine the best course of treatment for a speedy recovery.
If caught very early and treated properly, these sores can heal in a matter of days. If left untreated, severe bedsores may require years to heal.
Recommended Reading: Stelara Ulcerative Colitis Side Effects
Stage 4 Decubitus Ulcers
This is the most severe type of decubitus ulcer stage and has the deepest wound. Not only is the skin damaged, but joints, muscles and tendons around the skin can also be damaged and are often exposed. This deep open wound is a problem, because it leads to severe infections and diseases that can ravish the immune system of patients. Once the bone becomes infected during this stage, it can lead to death or the need for amputation.
The stages of decubitus ulcers progress quickly and must be managed before they reach stage 4. These sores are often preventable and measures must be taken to ensure that infection, death and amputation do not occur.
You May Like: Signs You Might Have An Ulcer