Overview Of Inflammatory Bowel Disease
and ulcerative colitis Ulcerative Colitis Ulcerative colitis is a chronic inflammatory and ulcerative disease arising in the colonic mucosa, characterized most often by bloody diarrhea. Extraintestinal symptoms, particularly arthritis… read more , is a relapsing and remitting condition characterized by chronic inflammation at various sites in the gastrointestinal tract, which results in diarrhea and abdominal pain.
Inflammation results from a cell-mediated immune response in the gastrointestinal mucosa. The precise etiology of inflammatory bowel disease unknown, but evidence suggests that the normal intestinal flora inappropriately trigger an immune reaction in patients with a multifactorial genetic predisposition . No specific environmental, dietary, or infectious causes have been identified. The immune reaction involves the release of inflammatory mediators, including cytokines, interleukins, and tumor necrosis factor.
How Does Ibd Affect Other Parts Of The Body
IBD can also cause problems outside the gut. Some people with IBD develop conditions affecting the joints, eyes or skin. These can be known as extraintestinal manifestations and often occur during active disease, but they can develop before any signs of bowel disease or during times of remission. Many of these are not very common.
JOINTS
Inflammation of the joints, often known as arthritis, is a common complication of IBD.
It is most common in those with Crohns Colitis and also affects about one out of 10 people with UC.
The inflammation usually affects the large joints of the arms and legs, including the elbows, wrists, knees and ankles. Fluid collects in the joint space, causing painful swelling, although pain may occur without obvious swelling. Symptoms usually improve with treatment of intestinal symptoms, and there is generally no lasting damage to the joints. A few people develop swelling and pain in the smaller joints of the hands or feet. This may be longer lasting and persist even when the IBD is in remission.
Sometimes, the joints in the spine and pelvis become inflamed a condition called ankylosing spondylitis . This can flare-up independently of IBD. It often causes pain over the sacroiliac joints, on either side of the lower part of the spine. Stiffness and pain in the spine itself may eventually lead to loss of flexibility.
SKIN
MOUTH
EYES
BONES
KIDNEYS
LIVER
Some complications are related to the liver and its function.
BLOOD CIRCULATION
ANEMIA
What Is The Prognosis Of Ulcerative Colitis With Extraintestinal Manifestations
Extraintestinal manifestations are common in ulcerative colitis approximately 25-35% of patients with inflammatory bowel disease have at least one extraintestinal manifestation. Extraintestinal disease may be prognostically important because the rate of pouchitis increases after colectomy in patients with UC and extraintestinal manifestations.
Pyoderma gangrenosum occurs in 1% of UC patients. An indolent chronic ulcer may occur even when disease is in remission. Intralesional therapy with steroids is useful, and colectomy results in healing in approximately 50% of patients.
Ophthalmologic manifestations most frequently occur when the disease is active. The incidence in adults is 4% but is less in children. The most common findings are episcleritis and anterior uveitis. Uveitis is usually symptomatic, causing pain or decreased vision. Patients with IBD should likely undergo routine ophthalmologic examination.
Arthritis is the most common extraintestinal manifestation of IBD, occurring in 10-25% of adolescents. The arthritis is usually a transient, nondeforming synovitis that involves the large joints in an asymmetric distribution. In children, arthritis may precede gastrointestinal symptoms by years.
References
Levine A, Griffiths A, Markowitz J, Wilson DC, Turner D, Russell RK, et al. Pediatric modification of the Montreal classification for inflammatory bowel disease: the Paris classification. Inflamm Bowel Dis. 2011 Jun. 17 :1314-21. .
Also Check: What Causes Venous Stasis Ulcers
Chronological Order Of Eims
Recent pediatric studies have shown higher rates of EIMs at IBD onset compared with adults . Greuter et al. also found that EIMs appeared before the initial diagnosis of IBD in up to 30% of pediatric patients with IBD. The specific EIMs that appeared before the IBD diagnosis were peripheral arthritis first, followed by uveitis, EN, axial arthropathy, and aphthous stomatitis. In this study, all cases of psoriasis and pyoderma gangrenosum appeared after an IBD diagnosis. Moreover, they found that peripheral arthritis and uveitis appeared significantly more frequently after versus before the diagnosis of IBD. The median lag of time of EIM appearance before the IBD diagnosis was 5.0 months . The study also investigated the chronological appearance of EIMs in pediatric patients with IBD before versus after the diagnosis, and the results showed that musculoskeletal symptoms, such as peripheral arthritis, were the most common first EIMs, followed by stomatitis, ophthalmological problems such as uveitis, and skin changes .
These results in children and adults with IBD suggest that awareness of the EIMs manifesting before gastrointestinal symptoms in IBD should help decrease the diagnostic delay in adult and pediatric patients with IBD.
Hepatobiliary Manifestations: Primary Sclerosing Cholangitis
PSC is the most important hepatobiliary manifestation of IBD because of its frequency, severity, and complex therapeutic approach. PSC is a chronic cholestatic liver disease of autoimmune etiology in which there is inflammation and fibrosis of the intra- and extrahepatic biliary ducts and that has a progressive course. The therapeutic arsenal currently available has a limited benefit in terms of modifying the natural history of the disease, with liver transplantation often being the only effective and definite treatment. Therefore, it is necessary to monitor patients with PSC rigorously, with the involvement of a multidisciplinary team of gastroenterologists, hepatologists, and endoscopists.
PSC is the most prevalent liver manifestation of IBD, with a frequency among cohorts varying from 0.6% to 10.5%. The disease predominantly affects men aged between 25 and 45 years. PSC is more associated with UC than with CD, and pancolitis is the intestinal pattern most frequently found in patients with UC .
Most patients with PSC are asymptomatic at the time of diagnosis, and the elevation of alkaline phosphatase levels is an important sign for diagnosis. Symptoms such as fatigue and pruritus may occur in the initial stages, and jaundice, choluria, acholic stools, hepatosplenomegaly, ascites, and encephalopathy may appear as the disease progresses . Episodes of infectious processes in cholangitis caused by bacterial infection secondary to obstruction may also occur.
Diagnosis
Recommended Reading: Best Probiotic For Ulcerative Colitis
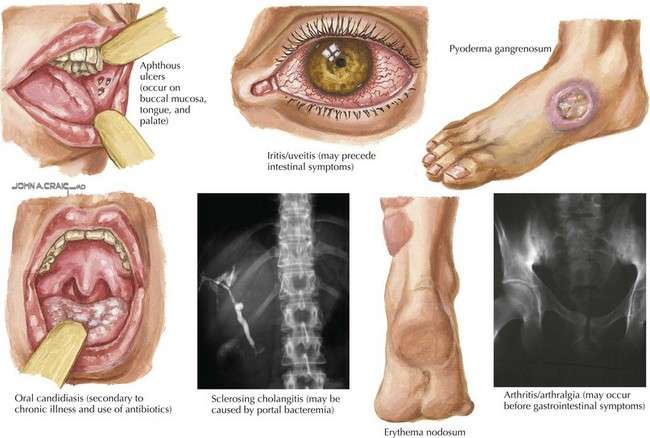
Extraintestinal Manifestations And Complications
Aphthous ulcersPyoderma gangrenosum
UC is characterized by immune dysregulation and systemic inflammation, which may result in symptoms and complications outside the colon. Commonly affected organs include: eyes, joints, skin, and liver. The frequency of such extraintestinal manifestations has been reported as between 6 and 47%.
UC may affect the mouth. About 8% of individuals with UC develop oral manifestations. The two most common oral manifestations are aphthous stomatitis and angular cheilitis. Aphthous stomatitis is characterized by ulcers in the mouth, which are benign, noncontagious and often recurrent. Angular chelitis is characterized by redness at the corners of the mouth, which may include painful sores or breaks in the skin. Very rarely, benign pustules may occur in the mouth .
UC may affect the eyes. Inflammation may occur in the interior portion of the eye, leading to uveitis and iritis. Uveitis can cause blurred vision and eye pain, especially when exposed to light . Untreated, uveitis can lead to permanent vision loss. Inflammation may also involve the white part of the eye or the overlying connective tissue , causing conditions called scleritis and episcleritis. Uveitis and iritis are more commonly associated with ulcerative colitis, whereas episcleritis is more commonly associated with Crohn’s disease.
Extraintestinal Complications Of Ibd
Inflammatory bowel disease can cause a variety of symptoms, both in the gut and out of the gut. When the disease affects other parts of the body, this is known as an extraintestinal manifestation or complication. Between 25-40% of IBD patients experience EIMs, commonly in the joints, skin, bones, eyes, kidneys, and liver. Anemia is another extraintestinal complication that IBD patients may experience.
Navigate the list below to learn more about the different potential extraintestinal complications of IBD:
You May Like: Is Nexium Good For Ulcers
The Difference In Extraintestinal Manifestations Of Inflammatory Bowel Disease For Children And Adults
Hyo-Jeong Jang1, Ben Kang2, Byung-Ho Choe2
1Department of Pediatrics, Keimyung University School of Medicine , 2Department of Pediatrics, School of Medicine, Kyungpook National University , South Korea
Contributions: Conception and design: All authors Administrative support: All authors Provision of study materials or patients: All authors Collection and assembly of data: All authors Data analysis and interpretation: HJ Jang, B Kang Manuscript writing: All authors Final approval of manuscript: All authors.
Correspondence to:
Abstract: Extraintestinal manifestations are frequently observed in adult and pediatric patients with inflammatory bowel disease . The most common EIMs involve the joints, skin, and eyes, but they can affect various organs and result in significant morbidity. Since EIMs can appear years before the diagnosis of IBD is made, clinicians should be aware of their various manifestations to help decrease diagnostic delay of IBD and establish appropriate treatment plans.
Keywords: Inflammatory bowel disease extraintestinal manifestations pediatric Crohns disease ulcerative colitis
Submitted Dec 22, 2018. Accepted for publication Jan 23, 2019.
doi: 10.21037/tp.2019.01.06
Table 1Table 2
Psc Is The Most Frequent Biliary Manifestation Of Ibd
It is more common in patients with UC than in CD. Approximately, 2.4% to 7.5% of patients with UC are diagnosed with PSC., Conversely, 75% of patients with PSC suffer from IBD, typically UC., PSC manifests with inflammation and fibrosis of the biliary system that presents clinically with a chronic cholestatic disease. A cholestatic biochemical profile is seen, and characteristic features are frequently found on cholangiography. These include multifocal bile duct strictures and segmental dilatation. PSC can precede the diagnosis of IBD however, some patients are even diagnosed with PSC several years after proctocolectomy due to UC.
Don’t Miss: Symptoms Of Intestinal Ulcers In Humans
Inflammatory Bowel Disease: Extraintestinal Manifestations
Extraintestinal manifestations of inflammatory bowel disease can complicate treatment regimens and reduce patient quality of life. An understanding of the clinical presentations and treatment options for this disease may aid in improving patient outcomes, according to an article published in Gastroenterology.
Unlike extraintestinal complications of IBD, EIMs are not a sequela of intestinal inflammation, and may present before or after the development of gastrointestinal symptoms. Evidence suggests the likelihood of developing EIMs is tied to genetic variants and smoking. The presence of EIMs is common in both ulcerative colitis and Crohn disease. The relationship between EIMs and immune system response, as well as microbiota, is hypothesized but requires more research.
Musculoskeletal EIMs, affecting up to 46% of patients with IBD, are the most prevalent type. Categorized within the spondyloarthritis family, there may be axial or peripheral involvement. Treatment of the underlying IBD often improves musculoskeletal EIMs, though symptoms may persist despite adequate control of intestinal inflammation.
Cutaneous, ocular, and hepatobiliary EIMs are present in up to 15%, 7%, and 5%, of patients with IBD, respectively. Episcleritis, a common ocular EIM, is closely tied to intestinal inflammation and treatment of the underlying IBD is key. Other manifestations, such as the cutaneous EIM pyoderma gangrenosum, require treatment independent of IBD control.
Reference
Presentation Of Disease At Diagnosis
Several attempts have been made in the past few years to define clinical presentation of late-onset UC and to determine if this variant may be different from adult forms.
Compared with adult-onset UC, more frequent weight loss but less frequent rectal bleeding and systemic symptoms like fever have been reported in older populations with UC onset . In particular, UC onset in older patients requires a careful diagnostic work-up to differentiate between drug-induced colitis , segmental colitis associated with diverticular disease, ischemic or infectious colitis or even neoplastic disease , and this may lead to the significant diagnostic delay reported in late-onset disease . Concerning disease extension at diagnosis , in a meta-analysis from 2016, left-sided colitis prevails in older-onset disease . This finding was confirmed by subsequent studies , whereas in other studies, extensive colitis or proctitis were more frequent in late-onset UC. Some studies found significant differences for disease extension at diagnosis between adult- versus late-onset UC , whereas others did not find such differences . Taken together, Fig. 1 depicts the most important studies in the past decade concerning disease extension at diagnosis including, where available, the corresponding figure of adult-onset UC.
Table 1 Comparison of the main features of ulcerative colitis at diagnosis and follow-up over 5 years, between adulthood-onset and late-onset diseaseFig. 1
You May Like: Foods You Can Eat With An Ulcer
What Is The Relation Between Extraintestinal Manifestations And Treatment Choice In Ibd
Runs 1:53
Extraintestinal manifestations of inflammatory bowel disease can substantially affect the morbidity associated with the disease, and some EIMs, such as primary sclerosing cholangitis or thromboembolic conditions, can increase mortality. The development of one EIM may increase the risk of additional EIMs. Many patients with EIMs have extensive colitis and may have a positive family history for IBD. EIMs are more common in patients with Crohns disease than in those with ulcerative colitis .
The frequency, type, and order of appearance of EIMs relative to IBD diagnosis was assessed in a 1249-patient cohort, of whom 366 had EIMs . The majority had only one episode. The first EIM was identified in 25.8% of patients at a median 5 months before IBD diagnosis. In 74.2% of patients the first EIM was seen at a median 92 months after IBD diagnosis. A finding of EIMs should prompt investigation for underlying IBD, as this can reduce delay in IBD diagnosis and may allow prevention of bowel damage.
Medical Therapyeffectiveness And Persistence
Every type of drug, from mesalazine through steroids, immunomodulators, and biotechnological therapies, used in adult UC are also indicated in older patients with UC limitations and contraindications depend on coexisting comorbidities. There is a lack of specific studies addressing efficacy of mesalazine, steroids, especially low bioavailability steroids, or immunomodulators in the older UC population. As shown by Kochar et al. in a recent systematic review , < 1% of patients included in randomized clinical trials were 65 years. The evidence reported in literature in real-life studies concerning effectiveness of available therapies and persistence in therapy is therefore summarized in Table 2, divided into late-onset and older patients with long-standing disease .
Table 2 Effectiveness of and persistence in therapies in patients with late-onset ulcerative colitis and with long-standing UC in comparison with younger adult patients unless otherwise indicated
You May Like: Meals For People With Ulcers
Renal And Pulmonary Manifestations
Nephrolithiasis, obstructive uropathy, and fistulization of the urinary tract are relatively common EIMs, occurring in 623% of patients with IBD. Secondary amyloidosis is a rare systemic complication that involves the kidneys. Patients can present with proteinuria, renal failure, and uremia. Studies have shown a 3-fold increased risk in males and a 10-fold increased risk in CD patients . In the majority of patients, other EIMs develop concurrently. A diagnosis can be made with a liver, rectal, or renal biopsy. Expedient renal transplantation in recent years has improved survival, although the survival rate after 15 years remains only 60%.
Finally, subclinical disturbances in lung function are common in IBD patients. Clinically significant disease is extremely rare. Chronic bronchitis, subglottic stenosis, bronchiectasis, and bronchiolitis have all been reported in association with IBD., These conditions can occur in nonsmokers and do not parallel bowel disease. Sulfasalazine and mesalamine can induce interstitial lung disease on rare occasions.
What Is The Overlap In Extraintestinal Symptoms Of Ulcerative Colitis And Crohn Disease
Ulcerative colitis and Crohn disease share many extraintestinal manifestations, although some of these tend to occur more commonly with either condition . Eye-skin-mouth-joint extraintestinal manifestations reflect active disease, whereas pyoderma gangrenosum, primary sclerosing cholangitis , ankylosing spondylitis, uveitis, kidney stones, and gallstones may occur in quiescent disease.
Although both ulcerative colitis and Crohn disease have distinct pathologic findings, approximately 10%-15% of patients cannot be classified definitively into either type in such patients, the disease is labeled as indeterminate colitis. Systemic symptoms are common in IBD and include fever, sweats, malaise, and arthralgias.
The rectum is always involved in ulcerative colitis, and the disease primarily involves continuous lesions of the mucosa and the submucosa. Both ulcerative colitis and Crohn disease usually have waxing and waning intensity and severity. When the patient is symptomatic due to active inflammation, the disease is considered to be in an active stage .
Recommended Reading: What Is Peptic Ulcer Disease
Extraintestinal Manifestations Of Inflammatory Bowel Disease: Clinical Aspects And Pathogenesis
Sandro da Costa Ferreira*, Bernardo Bezerra Martins de Oliveira, André Marussi Morsoletto, Ana de Lourdes Candolo Martinelli, Luiz Ernesto de Almeida Troncon
Division of Gastroenterology, Department of Medicine, School of Medicine of Ribeirão Preto, University of São Paulo, Ribeirão Preto, Brazila
- Corresponding Author:
- School of Medicine of Ribeirão PretoUniversity of São PauloE-mail:
Accepted Date: January 18, 2018
Citation: Ferreira SDC, Oliveira BBMD, Morsoletto AM, et al. Extraintestinal manifestations of inflammatory bowel disease: Clinical aspects and pathogenesis. J Gastroenterol Dig Dis. 2018 3:4-11.
Visit for more related articles at
Prevalence Of Extraintestinal Manifestations In Korean Inflammatory Bowel Disease Patients
-
Roles Conceptualization, Investigation, Writing original draft
Affiliation Medical Research Collaborating Center, Seoul National University Hospital, Seoul, Republic of Korea
-
Affiliation Department of Health Convergence, Ewha Womans University, Seoul, Republic of Korea
- Mi-Sook Kim,
Roles Formal analysis, Methodology
Affiliations Medical Research Collaborating Center, Seoul National University Hospital, Seoul, Republic of Korea, Department of Preventive Medicine, Seoul National University College of Medicine, Seoul, Republic of Korea
- Jaeyoung Chun,
Roles Conceptualization, Writing review & editing
Affiliation Department of Internal Medicine and Liver Research Institute, Seoul National University College of Medicine, Seoul, Republic of Korea
-
Affiliation Division of Rheumatology, Department of Internal Medicine, Seoul National University Hospital, Seoul, Republic of Korea
-
Affiliation Medical Affairs, Janssen Korea, Seoul, Republic of Korea
Don’t Miss: Is Alcohol Bad For Ulcerative Colitis