Special Devices That Can Help You
In addition to turning and repositioning frequently, using a special surface to reduce or relieve pressure can help a great deal. The simplest of these is an egg crate mattress. Many hospice and home health agencies provide these free of charge but they are relatively inexpensive at your local department store.
If your loved one is spending a lot of time up in a chair, egg crate chair pads are also available. An egg crate surface helps distribute pressure more evenly, helping minimize the amount of pressure on one area.
A step up from the egg crate mattress is an air mattress overlay. This type of surface is placed on top of a mattress and typically alternates air pressure in various columns. When using an egg crate mattress or an air mattress overlay, its still important to maintain the turning schedule. These devices dont replace frequent repositioning.
The big guns of pressure-relieving devices are the fluidized air mattresses. These special mattresses contain silicone-coated glass beads that become fluid when the air is pumped through them. These mattresses do a wonderful job of relieving pressure but they have their downside.
The frame of the mattress makes transferring to and from bed difficult. And if the person wants to sit up in bed, a foam wedge would probably need to be used to help support their back. This mattress is really best suited for palliative care patients who are fully bed-bound, have severe pressure ulcers, and are in a lot of pain.
Daily Skin Care To Prevent Pressure Sores
Ways to prevent pressure injuries include:
- Checking the skin at least daily for redness or signs of discolouration.
- Keeping the skin at the right moisture level, as damage is more likely to occur if skin is either too dry or too moist.
- Using moisturising products to keep skin supple and prevent dryness.
- Never massaging bony areas because the skin is too delicate.
Caring For A Pressure Sore
Stage I or II sores will often heal if cared for carefully. Stage III and IV sores are harder to treat and may take a long time to heal. Heres how to care for a pressure sore at home.
Relieve the pressure on the area.
- Use special pillows, foam cushions, booties, or mattress pads to reduce the pressure. Some pads are water- or air-filled to help support and cushion the area. What type of cushion you use depends on your wound and whether you are in bed or in a wheelchair. Talk with your health care provider about what choices would be best for you, including what shapes and types of material.
- Change positions often. If you are in a wheelchair, try to change your position every 15 minutes. If you are in bed, you should be moved about every 2 hours.
Care for the sore as directed by your provider. Keep the wound clean to prevent infection. Clean the sore every time you change a dressing.
Avoid further injury or friction.
- Powder your sheets lightly so your skin doesnt rub on them in bed.
- Avoid slipping or sliding as you move positions. Try to avoid positions that put pressure on your sore.
- Care for healthy skin by keeping it clean and moisturized.
- Check your skin for pressure sores every day. Ask your caregiver or someone you trust to check areas you cant see.
- If the pressure sore changes or a new one forms, tell your provider.
Take care of your health.
You May Like: Can I Take Tylenol For Stomach Ulcer Pain
Read Also: What Is A Venous Ulcer
Prevention Of Heel Pressure Injuries
The geometry, anatomy, and perfusion of the heel create challenges in preventing HPIs. International guidelines suggest that to redistribute pressure from the heel, the heel should be floated from the bed. Suspending or floating the heels clear off the support surface by elevating the lower leg or calf is demonstrated to be an effective strategy to relieve pressure, shear, and friction forces, thereby reducing the risk of HPIs. Unfortunately, floating the heel on pillows does not always work if the patient moves about in bed or the pillow collapses from the weight of the leg. In addition, floating the heels will always result in greater weight bearing in other anatomical areas and may shift the risk for injury to elsewhere in the body. When determining which mechanism to use to offload the heel, consider the following issues: How long will the legs be immobile, and how mobile is the patient? Is the patient agitated and moving a lot? Is there poor arterial flow? Are there sensory limitations such as paraplegia or neuropathy? Is the patient is ambulatory? Does the patient slide down in the bed, or do they need a bed extender?
Considerations in Elevating the Heels2
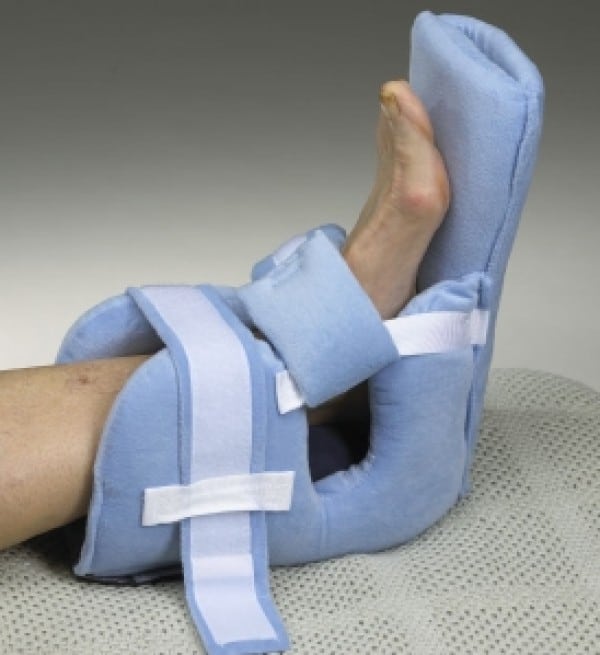
Systam Memory Foam Pressure Relief Heel Boot
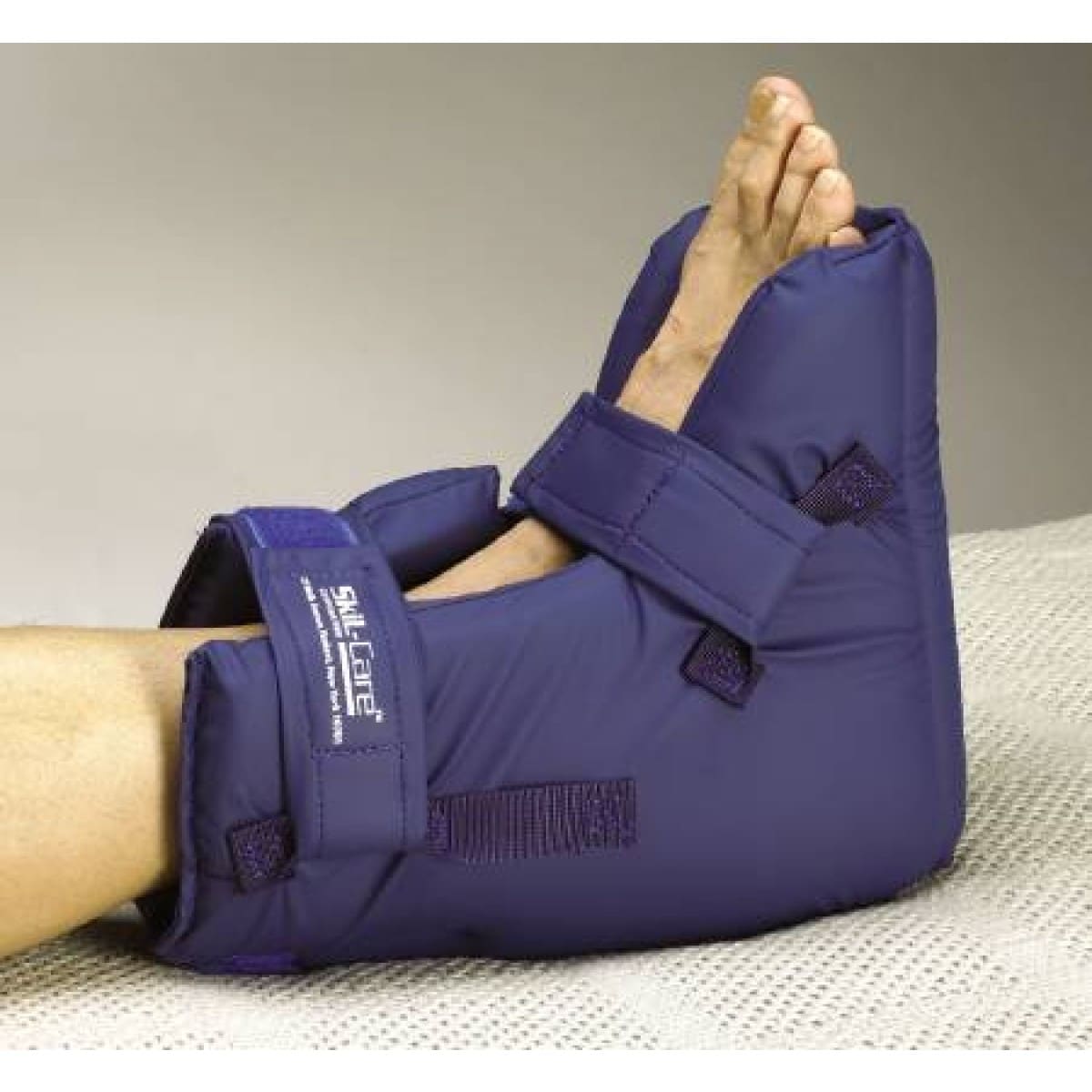
For patients at particularly high risk of pressure sores, or for those already suffering from ulcers, more serious measures may be necessary. Suited to post-surgical recovery or patients in intensive care, the Systam Memory Foam Pressure Relief Heel Boot provides powerful pressure relief with moulded memory foam that is shaped to prevent equinus distortion and rotation a particularly heinous risk factor for pressure sores.
The zone at the base of the heel is completely cut away, enabling the heel to be entirely suspended for complete relief of pressure. A valley on the boot prevents excess pressure on the achilles tendon, making the boot a complete pressure relief solution for the lower legs.
Key Features: Moulded with foam to completely suspend the heel, prevents rotation for powerful and all-encompassing pressure relief.
You May Like: Best Diet For Gerd And Ulcers
Don’t Miss: What Can You Do For An Ulcer In Your Mouth
Summary Of Included Studies
| Landi 2003 | Nerve growth factor Placebo | People in a nursing home with a stage 2 to 5 foot pressure ulcer |
|
|
| Meaume 2009 | 10g sachet of ornithine alpha-ketoglutarate versus 1 sachet of placebo | Elderly people who had pressure ulcers of the heel of stage 2 or 3 |
|
6 weeks |
| Female inpatients with a grade 4 heel pressure ulcer |
|
|||
| Russell 2000 | 2 types of alternating cell mattress systems with pressure-relieving cushions: Huntleigh Nimbus 3 with Aura cushion and 4-hourly turning versus Pegasus Cairwave Therapy System with Proactive 2 seating cushion and 8-hourly turning. | People from care of the elderly units with pressure ulcer of grade 2 or above . Average age 83.9 and 84.6 years in the 2 groups. |
|
18-month follow-up |
Clinical evidence profile: ornithine alpha-ketoglutarate versus placebo.
ANCOVA used. Non-parametric tests detected between-group differences which were confirmed by parametric tests after log-transformation to normalise distribution .
Contributions Of Editorial Base:
Nicky Cullum: advised on methodology, interpretation and protocol content. Julie Bruce, Editor: approved the final protocol prior to submission. Sally BellSyer: coordinated the editorial process. Advised on methodology, interpretation and content. Edited the protocol. Ruth Foxlee: designed the search strategy and edited the search methods section.
Read Also: Best Iron Supplement For Ulcerative Colitis
Floating Heels: More Than Just Pillow Talk
The way you float the heels matters: new guidelines mean better patient care and lower risk of citations.
When it comes to wound care, the term float the heels means that a patients heel should be positioned in such a way as to remove all contact between the heel and the bed. So given this context, is the following statement true or false?
Patients on support surfaces do not require their heels to be floated.
If you guessed false, then give yourself a gold star. Yes, all patients at risk of breakdown, and those with pressure ulcers on the heel, must have their heels totally offloaded. This requirement has not changed.
But heres the catch what has changed is the manner in which we should be accomplishing this.
How Can Pressure Injuries Be Prevented
The development of pressure injuries can be prevented through careful observation of the skin and frequent repositioning in those who canât turn themselves. Tips to prevent pressure injuries include:
- Keeping the skin clean and clear of bodily fluids.
- Moving and repositioning the body frequently to avoid constant pressure on bony parts of the body.
- Using foam wedges and pillows to help relieve pressure on bony parts of the body when turned in bed.
- Maintaining a healthy diet to avoid malnutrition and to assist in wound healing.
Read Also: How Do You Get Ulcerative Colitis
What Are The Risk Factors For Pressure Ulcers:
People with fragile skin are at additional risk, as are people whose nutrition is poor. Diabetes is also a significant risk factor for pressure sores on the feet.
One of the reasons pressure sores are so common among the disabled is that many such people have impaired sensation of pressure and touch due to spinal cord injuries. Because of this, they may not be alerted by pain or discomfort to the need to change position.
People who are bedridden for extended periods may lose a great deal of weight, which reduces the cushioning around their bones, making them more susceptible to pressure sores.
Description Of The Condition
Pressure ulcers are defined as âa localized injury to the skin and/or underlying tissue usually over a bony prominence, as a result of pressure, or pressure in combination with shearâ . Pressure ulcer classification systems provide a method by which the depth and severity of the injury can be described and documented . Pressure ulcers have traditionally been categorised according to severity, from a category I pressure ulcer of intact skin) up to category IV . However, recently two additional categories have been defined âunstageable/unclassifiedâ and âsuspected deep tissue injuryâ . As pressure ulcers are categorised according to depth of the wound, these categories are used when the depth of the wound is unknown. The âunstageableâ category describes wounds in which slough or necrosis obscures the wound bed. âSuspected deep tissue injuryâ describes wounds in which it is suspected that there is deeper damage, such as when bruising or a blood blister is present. Although these additional categories were initially described for use in the USA, they have started to be used and investigated worldwide .
Why is the heel such a high risk area?
Recommended Reading: Colon Cleanse For Ulcerative Colitis
Read Also: Signs Of Ulcerative Colitis In Adults
Nurse Teaching On How To Prevent Pressure Ulcer Development
Pressure ulcers, also called bedsores, are injuries to skin and underlying tissue resulting from unrelieved and prolonged pressure on the skin. Pressure ulcers often develop in individuals with history of prolonged bedrest, wheelchair bound status, and limited independence for ADL performance. Bedsores develop secondary to the unrelieved pressure on the skin and the skin getting damaged between the dependent surface and the underlying bone. Pressure ulcers mostly develop on the skin over bony prominences, especially on the dependent parts of the body, such as, the elbows, shoulder blades, heels, ankles, hips, sacrum, and back of arms and legs resting against any surface for prolonged periods of time. Depending on the extent and depth of skin injury, pressure ulcers are graded into stages 1 4, 1 being mild injury and 4 being extensive injury to the skin involved. Pressure ulcers can be prevented by following some management techniques and it is important for individuals who are prone to having them to learn how to prevent pressure ulcer development. In this post we discuss some management measures that individual can learn regarding how to prevent pressure ulcer development.
How to prevent pressure ulcer development
Skin Status And Presence Of Pressure Ulcers
The presence of a category 1 pressure ulcer is correlated with a two-to-threefold increase in a patients risk of developing a more severe pressure ulcer . The presence of scar tissue and the presence of dry, thin or oedematous skin also increase the pressure ulcer risk. Ageing has been found to increase the risk of pressure ulcers due to the thinning of the epidermis as part of the normal ageing process . Ageing also causes the skin to become dehydrated and lacking in sebum , connective tissue to lose its elasticity and strength, and blood vessels to become increasingly fragile . Furthermore, subcutaneous tissues become thinner with age, which reduces the already minimal padding over the calcaneus and reduces the heels capacity to absorb shock .
Read Also: Stomach Ulcer And Chest Pain
Prevention Of Heel Pressure Ulcers
Because the development of a pressure ulcer is rarely due to a single causative factor, prevention strategies involve the nurse identifying each patients individual risk factors, as described previously for example, immobility, skin status, presence of pressure ulcers and/or scar tissue, and suboptimal tissue perfusion. This should involve a holistic risk assessment along with a thorough skin assessment. The signs of pressure damage that the nurse should look for when examining a patients heels include any signs of redness, and whether the skin blanches . It is not always possible to identify redness on darkly pigmented skin, so the nurse should assess for other signs of pressure damage including localised heat, oedema, blistering and induration .
In the UK, NICE states that patients in NHS secondary or long-term care must undergo a pressure ulcer risk assessment within six hours of admission . If a patient is found to be at risk of pressure ulcers, a preventive care plan should be initiated.
Official Floating Heels Guidelines
Traditionally, the most common approach to floating heels has been by placing pillows under the lower leg, positioned so as not to place pressure on the Achilles tendon and the heel. Unfortunately, there has always been a problem with this method.
While you might position your patients perfectly in bed, with heels properly floated, the chances that theyll remain perfectly still once youre gone is slim to none. Patients naturally move and reposition themselves for comfort, which means upon returning, you will most likely find that the legs and heels are no longer in that same position.
This repositioning is a common occurrence, and leaves your patients vulnerable to the forces of friction, shear and pressure on the heel. This traditional heel-floating technique often leads to unnecessary heel breakdown, and a failure to protect our patients properly. Additionally, facilities may be cited for floating Stage III heel ulcers on a pillow.
So whats the official word on the subject? The 2014 International Guidelines on the Prevention and Treatment of Pressure Ulcers tell us that:
- You can continue to float the heels with pillows under the full length of the calf for short-term use in alert and cooperative individuals.
- For individuals with Stage I or II pressure ulcers on the heel, you can float the heels, or use a heel suspension device.
- For individuals with Stage III, Stage IV or Unstageable pressure ulcers, heel suspension devices are strongly recommended.
Also Check: How To Diagnose Gastric Ulcer
Significance Of The Heel As A High
After the sacrum, the heel is frequently reported as the second most common site for the development of pressure ulcers, as well as the site where the most severe pressure ulcers tend to develop . Heel pressure ulcers can cause pain, reduce mobility and in severe cases result in amputation . Heel pressure ulcers can be challenging to heal. In a cohort of 140 patients with heel pressure ulcers categorised as category 2 or above recruited to a prospective cohort study in one large teaching hospital in the UK, only 42% were reported to have healed over the 18-month study period .
Figure 1.
Anatomy of the heel
TIME OUT 2
Do the risk assessments used in your clinical area include risk factors for pressure ulcers? What do you need to consider in your risk assessment to identify patients who are at high risk of developing pressure ulcers on the heel?
Preventing Heel Pressure Ulcers
Heels are particularly vulnerable to skin breakdown due to the fact that the posterior heel is covered only by a thin layer of skin and fat. When patients lie supine, all of the pressure of their lower legs and feet rest on the heels, which have relatively poor skin perfusion and a paucity of muscle tissue to absorb stress.
Prevalence rates for heel pressure ulcers vary, but have been estimated to be as high as 25% across a mixture of continuing care and acute care settings. Heel ulcers represent approximately 1/3 of pressure ulcers acquired, resulting in increased morbidity and mortality. In some cases, heel pressure ulcers can lead to amputation of the affected limb.
Don’t Miss: Alginate Dressings For Venous Leg Ulcers
Express Comfort Contoured Gel Foam Wheelchair Cushion
The Express Comfort Contoured Gel Foam Wheelchair Cushion by the Comfort Company offers a cooling sensation, which not only improves someoneâs comfort but it allows the skin to breathe better while seated. The gel is one of the most sought-after materials for pressure relief cushions, since people find them to be optimally durable and accommodating.
Donât Miss: How To Treat Pressure Ulcers On Buttocks
Reduce Friction And Shear
Friction is the rubbing of skin on an external surface, usually bed sheets. Friction to the most commonly affected areas can be reduced with protective devices. Heel and elbow cradles are typically made of egg-crate material and Velcro on.
Skin protecting dressings, such as films and thin hydrocolloid bandages can protect the skin from repeated friction but wont help reduce pressure.
The most important thing you can do to prevent injury from the friction is to make sure you dont create any yourself when youre repositioning your loved one. Use a draw sheet to help you lift your loved one off the bed when you lift and reposition.
Shear is created when the deeper fatty tissues and blood vessels are damaged by a combination of friction and gravity. The best way to avoid this type of injury is to avoid a semi-Fowler and upright position in bed. A semi-fowler position is where the head is raised less than 30 degrees and upright positions more than 30 degrees.
Now, you obviously cant avoid these positions all of the time. Many patients need to be semi-Fowler to help ease shortness of breath or prevent gastric reflux and all patients need to be in an upright position to eat safely.
To minimize the risk of shear injury in a semi-Fowler or upright position, take precautions to prevent your loved one from sliding down in bed. You can do this by raising the foot of the bed and propping the knees up with pillows.
Don’t Miss: Oats For Horses With Ulcers