Choosing The Right Diet For Ulcerative Colitis
Because each body is different, there isnt a one-size-fits-all diet for UC. Work closely with a registered dietitian to design a diet that works for you, Diekman advises. Its also good to keep track of what you eat in a food journal. This makes it easier to pinpoint which ingredients trigger your symptoms.
Additional reporting by Kaitlin Sullivan
Also Check: What Foods Are Good For Ulcers And Gastritis
Outcome And Complications From Ileoanal Anastomosis
Complications are common with any intestinal operation. In a small percentage of IPAA procedures, complications occur that require conversion to an ileostomy.
Pouchitis
Inflammation of the pouch is the most common complication of the pouch procedures. Symptoms include rectal bleeding, cramps, and fever. It can usually be successfully treated with antibiotics such as metronidazole or ciprofloxacin .
Bowel obstruction
Bowel obstruction may occur although it is less common than pouchitis. With most people, this condition can be treated by avoiding food for several days and administering intravenous fluids. In some cases of bowel obstruction, surgery may need to be performed to remove the blockage.
Pouch failure
Pouch failure occurs in a small percentage of people. It requires permanent removal of the pouch and use of ileostomy.
Irritable Pouch Syndrome
Irritable pouch syndrome is a problem that includes frequent bowel movements, an urgent need to defecate, and abdominal pain. However, there are no signs of inflammation as there are with pouchitis. Stress and diet play a role in this condition, and it is usually relieved after a bowel movement.
Infertility
IPAA can cause infertility in women because the surgery can scar or block the fallopian tubes.
Youre Not Drinking Enough Fluids
If youre experiencing a bout of diarrhea, you run the risk of becoming dehydrated because your body is losing more fluids than its taking in. This can be harmful to your overall well-being and interfere with your bodys ability to heal.
Drink as much water as you can during a UC flare. Just keep in mind that there are some liquids you should think twice about if you have diarrhea, including pear, peach, or prune juice, according to the Crohns and Colitis Foundation all of them contain nonabsorbable sugars that can be rough on your gut.
You May Like: Turn Clock For Pressure Ulcer Prevention
What Side Effects Of Ibd Can Cause Malnutrition
There are several reasons why people with IBD may be at risk for malnutrition. The following list includes some side effects that contribute to malnutrition.
- Inadequate food/fluid intake may by caused by nausea, abdominal pain, loss of appetite or altered taste sensation
- Increased losses â intestinal inflammation during acute flares results in increased protein losses, losses from fistula fluids, diarrhea and bleeding
- Increased nutritional needs â inflammation or infection increases metabolic requirements
- Malabsorption with Crohn’s disease may be caused by severe intestinal inflammation, resection of small intestine and medications, such as prednisone and sulfasalazine
The Best Foods To Eat And Avoid For Inflammatory Bowel Disease
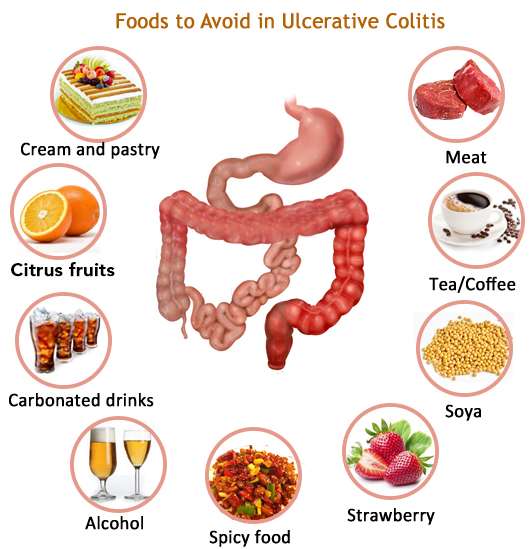
Inflammatory bowel disease is a treatable, yet chronic and lifelong condition. IBD is a broad term that refers to the inflammation of the gastrointestinal tract and includes specific conditions such as ulcerative colitis and Crohns disease.
No plan has been proven to prevent or control IBD. But managing your diet can help manage your disease during flares and periods of remission. Be sure to talk to your physician or a registered dietitian about your nutrition needs and managing IBD.
Here are diet recommendations for managing IBD flares and remissions from UH Outpatient Nutrition Services.
Read Also: Difference Between Ulcerative Colitis And Crohn’s Disease Ppt
Commercial Meal Replacement Shakes And Protein Powders
Commercial meal replacement shakes are intended to provide a person with important nutrients and boost their calorie intake. Commercial protein powders may be helpful if you have a hard time getting enough protein from the food you eat. One MyCrohnsAndColitisTeam commenter said, Boost and Premier protein meal replacement shakes have often been the only things that will stay in my tummy, along with oatmeal.
How Is Ulcerative Colitis Treated
Theres no cure for ulcerative colitis, but treatments can calm the inflammation, help you feel better and get you back to your daily activities. Treatment also depends on the severity and the individual, so treatment depends on each persons needs. Usually, healthcare providers manage the disease with medications. If your tests reveal infections that are causing problems, your healthcare provider will treat those underlying conditions and see if that helps.
The goal of medication is to induce and maintain remission, and to improve the quality of life for people with ulcerative colitis. Healthcare providers use several types of medications to calm inflammation in your large intestine. Reducing the swelling and irritation lets the tissue heal. It can also relieve your symptoms so you have less pain and less diarrhea. For children, teenagers and adults, your provider may recommend:
Children and young teenagers are prescribed the same medications. In addition to medications, some doctors also recommend that children take vitamins to get the nutrients they need for health and growth that they may not have gotten through food due to the effects of the disease on the bowel. Ask your healthcare provider for specific advice about the need for vitamin supplementation for your child.
You might need surgery that removes your colon and rectum to:
- Avoid medication side effects.
- Prevent or treat colon cancer .
- Eliminate life-threatening complications such as bleeding.
Don’t Miss: What To Eat With An Ulcerative Colitis Flare Up
Youre Avoiding Certain Healthy Foods
It can be hard to eat a healthy diet or anything at all if youre experiencing abdominal pain, cramps, or nausea. But if youre not eating the right foods, you could be at risk of nutrient deficiencies, malnutrition, and unwanted weight loss.
While theres no one meal plan that works for everyone, many people find they can tolerate low-fiber fruits , lean proteins, cooked veggies, and grains like sourdough and oatmeal. A doctor or dietitian who specializes in IBD can help you develop a personalized meal plan.
What Is The Diet
Although theres a lot of existing research on the relationship between food and UC, no one diet has been shown to consistently reduce the underlying inflammation thats found in adults with this condition. Some studies suggest that UC flares are associated with the consumption of red or processed meat, dairy products, coconut oil, palm oil, artificial sweeteners, and/or certain food additives. However, avoiding these foods may help improve symptoms of the disease, but reducing actual inflammation is best achieved with medical therapies, advises Dr. Hong.
Read Also: How Severe Is Ulcerative Colitis
Turmeric And Ginger Tea
Turmeric, a relative of ginger, has been used in Ayurvedic medicine for millennia to help treat inflammatory diseases. Curcumin, the active component of turmeric, may be a safe, effective therapy for maintaining or inducing UC remission when administered with standard treatments, according to a review published in July 2020 in Nutrients. Try this soothing concoction submitted by nascarrunner71 at AllRecipes.com: Hot or cold, this tea combines ginger, turmeric, and honey or maple syrup for a rich and flavorful tea.
Ive Been In Your Shoes
I remember what its like to be in my early 20s where I hit the club like 3-4 times a week. It can be difficult to go out with your friends and feel like the odd ball. You might slip up and I wrote this article to help you get through these times.
Remember youre playing the long game right now, which is to achieve long term remission. Once you heal your gut you can be less strict. I believe that once you experience what it feels like to feel truly awesome, you wont care about being like everyone else.
You May Like: Wound Care For Diabetic Leg Ulcers
It Doesnt Have To Be Chronic
The latest research shows that combining herbal compounds like curcumin and qing-dai with standard medication can quickly induce remission in patients, including those who were non-responsive to drug therapies.
The European Crohns and Colitis Organization lists Curcumin as an effective add-on therapy to 5-ASA in in-ducing remission in mild-to-moderately active ulcerative colitis
A peer-reviewed study led by our founders and published in the prestigious Clinical Gastroenterology and Hepatologyjournal found gut-directed curcumin to be effective in inducing clinical and endoscopic remission when combined with mesalamine in patients with mild-to-moderate colitis.
A systematic review published in Journal of Complementary Therapies in Medicine found that curcumin re-duced inflammatory markers and disease activity in patients with Crohns disease. They also indicated curcumin re-duces the level of an inflammatory molecule called IL-1, which is believed to be involved- at least partly in loss of re-sponse to biological agents. The researchers, coming from Grand Valley University in Michigan, suggested that adding curcumin may prove to be beneficial, and concluded that Curcumin, even by itself, was found to be a cheap and safe way to reduce Crohns disease symptoms and inflammatory markers.
Curcumin add-on treatment maintains remission 4X better than pharmaceutical treatment alone
You May Like: Is Oatmeal Good For Ulcerative Colitis
Ibds And Alcohol: What To Drink And What Not To Drink

People think that if you have an Inflammatory Bowel Disease like Crohns Disease or Ulcerative Colitis that you shouldnt take a sip of alcohol. In a perfect world that might be the case. In reality, most of our social interactions revolve around some form of drinking. Not having a drink isnt always an option.
I get it, you want to have fun with your friends, feel like you fit in, and there is nothing wrong with that. Im writing this article because like you Im a human being. I enjoy having a drink and I want you to be able to do the same. Pretending that someone with an IBD will never have a drink is completely naive!
The key is learning what you can do to minimize or eliminate negative side effects.
Recommended Reading: Can You Have An Ulcer In Your Colon
Herbal Remedies And Supplements
There are lots of supplements that claim to treat Crohns and Colitis. But there isnt enough evidence to recommend any herbal remedies or supplements. This is because its difficult to know whether the supplement is directly affecting a persons Crohns or Colitis or whether something else is causing a change in symptoms. Also, everyone is different so what helps one person may not help another.Some people find that some herbal remedies, such as aloe vera or curcumin , help them manage their symptoms when they use them together with their prescribed medicines. There have been reports of cannabidiol , an ingredient in cannabis, helping with symptoms like diarrhoea, pain and loss of appetite. But we dont know enough about how it works or how much is a safe amount to take. It isnt currently recommended and isnt available on prescription for people with Crohns or Colitis.There have been claims in the media about the benefits of kefir a fermented milk drink that contains probiotics. But there isnt any medical evidence to show that it helps people with Crohns or Colitis.If you want to take herbal remedies, its important to speak to your IBD team or dietitian first. Dont stop taking your prescribed medicine without talking to your IBD team, even if your symptoms improve.
I think it is so important to remember that the relationship with food and IBD is so different for everyone!
What Foods Should I Not Eat When I Am Having An Ulcerative Colitis Flare
Certain foods can exacerbate or aggravate an UC flare and should be avoided. They are more likely to trigger cramping, bloating, and/or diarrhea and are also not recommended in people diagnosed with a stricture, which is a narrowing of the intestine caused by inflammation or scar tissue, or in those who have had recent surgery. Examples include:
- Foods high in insoluble fiber that are hard to digest, such as seeds, raw green vegetables , whole nuts, whole grains, or fruits with a skin
- Lactose, which is milk sugar found in dairy products, milk, cream, cream cheese, and soft cheeses
- Non-absorbable sugars such as sorbitol, mannitol, and other sugar alcohols that are typically found in sugar-free gum, candy, ice cream, and certain types of fruits and juices such as pear, peach, and prune juice
- Sugary foods such as candy, pastries, and juices
- High-fat foods such as butter or margarine, coconut oil, or fatty, fried, or greasy food
- Spicy foods
- Alcohol such as beer, wine, or spirits
- Caffeinated drinks such as coffee or energy drinks
- Soda.
Don’t Miss: Nasal Cannula Pressure Ulcer Prevention
How To Stay Hydrated In Spite Of Ibd
When people think about staying hydrated, they often just think of drinking lots of water, but that can be difficult for someone with Crohnâs disease or ulcerative colitis when theyâre not feeling well or in a flare. It is still very important that we stay hydrated as our bodies depend on those fluids to keep us healthy.
7 Tips to Help you Stay Hydrated: :
- Take frequent small sips if you donât feel like guzzling large amounts
- Set a timer and drink whatever you can every hour or half-hour
- Drink the water at the temperature you like. Add a cool glassful in the morning, ice-cold water later and / or a cup of hot water with lemon in the evening.
- Fill a bottle or glass of water and keep it with you. Use the container size that appeals to you the most. Some people like to have a huge mug next to them, but that can intimidate others.
- Drink your favorite beverages . Just be mindful about added sugars!
- Eat foods high in fluid content
- Infuse your water with slices of fresh fruit, cucumber, or a squeeze of fruit juice
Stay Away from Salt, Alcohol and Excess Sugar and Protein
- Salt holds onto the water, so you donât get to use it so avoid salty snacks, canned soups, deli, and frozen dinners
- Alcohol dries out the cells, so avoid it or alternate with extra fluid
- Excess Protein and Sugar can require extra fluid to eliminate them though the kidneys
This article, as well as all others, was reviewed and edited by a member of our Medical Advisory Board.
Can You Eat Tuna With Colitis
Fatty foods can trigger increased abdominal pain and gas, so many people with ulcerative colitis avoid fatty cuts of meat and focus on lean sources of protein, such as poultry, instead. Salmon and tuna are exceptions to the rule. These fish are high in omega-3 fatty acids, a type of fat that may reduce inflammation.
You May Like: Treating Leg Ulcers With Sugar
Avoiding The Negative Effects Of Alcohol
If you have a hard time controlling your alcohol consumption, ulcerative colitis may not be the only condition that you are at risk for. Chronic alcohol abuse is linked to higher rates of heart disease, other forms of IBDs, higher chances of accidents, and decreased mental health.
Even if you know of alcohols negative effects, it can be hard to quit. To improve your drinking habits and your overall quality of life, you may want to look at alcohol treatment options.
To find the best alcohol abuse treatment available for you or your loved one, contact us today.
The Worst Foods For Those With Ulcerative Colitis
Ulcerative colitis is an inflammatory chronic disease of the colon and rectum where ulcers develop inside the lining of the large intestine. It is an inflammatory bowel disease along with Crohns Disease which causes a multitude of painful and unpleasant symptoms. Since dietary habits can contribute to ulcerative colitis symptoms, lets look at the worst foods for those with ulcerative colitis.
Don’t Miss: Can Food Allergies Cause Ulcerative Colitis
Water Is The Best Thing To Drink For People With Crohns Disease
It may not sound exciting, but the best hydration when managing an IBD such as Crohns disease is plain H2O. Theres no other beverage that will work harder to help you overcome the negative effects of Crohn’s symptoms, experts say. This is especially true when diarrhea strikes and your fluid needs are even greater.
What To Eat During Flare
Low-fiber foods are easiest to digest and are less irritating to the gut, especially with symptoms like abdominal pain or diarrhea. Choose:
- Grains/starches: White foods, instead of wheat or whole-grain, and those with less than 2 grams of fiber per serving
- Cooked vegetables: Well-cooked vegetables such as green beans, carrots, mashed potatoes without skin, steamed asparagus tips and pureed squash.Use fresh or frozen.
- Canned or soft fruits: Peeled apples, ripe bananas, cantaloupe, honeydew, watermelon, and canned fruit in fruit juice or light syrup
Be sure to eat enough protein — Inflammation causes increased protein needs. Choose:
- Tender, well-cooked meats: Poultry, salmon or other fish, lean beef and pork prepared without added fat
- Deli meats: Low-sodium and low-fat varieties
- Eggs: Well-cooked
- Tofu
- Smooth nut and seed butters: Peanut, almond or sunflower seed
Drink plenty of fluids — Aim for eight cups a day, and consider using oral rehydration beverages as needed. Try to limit caffeinated, sugar drinks and beverages made with sugar substitutes.
Limit added fats and oils — Focus on oils instead of solid fats, and limit intake to less than eight teaspoons per day.
Consume adequate calcium, vitamin D, probiotics, and prebiotics — Sources include:
Also Check: What Is Stomach Ulcer Pain Like
Lifestyle Changes To Prevent Ulcerative Colitis
Dealing with colitis flare-up can be approached different ways. Some people have reported that herbal remedies help manage their symptoms. Probiotics, the spice turmeric, and the herb boswellia have been used to control ulcerative colitis. Studies have also shown that gingko biloba has been effective in treating colitis in rodents.
Since stress has been linked to the disease, exercises like yoga and meditation are often recommended to patients. At the same time, certain foods have a higher chance of aggravating ulcerative colitis, so obviously avoiding such food items is a good idea. Some examples of foods to stay away from are whole-grain bread, whole-grain pasta, beans, raw vegetables, and dried fruit. Keeping a diary of what you eat can often help you pinpoint the exact cause of a flare-up.
A diary or journal can also help when you are taking medications. For example, if you experience a flare-up while taking an over-the-counter medication, ask your doctor and/or pharmacist about a possible alternative.
Controlling ulcerative colitis flare-up can take time. Some people will have multiple triggers and wont be able to make all the necessary lifestyle adjustments all at once. Sometimes, just a few changes can make a huge difference though. The following simple steps have proven to help many people tame their flare-ups:
- Drinking small amounts of water throughout the day
- Reducing fatty foods