What Are The Clinical Features Of Diabetic Foot Ulcer
A diabetic foot ulcer is a skin sore with full thickness skin loss often preceded by a haemorrhagicsubepidermal blister. The ulcer typically develops within a callosity on a pressure site, with a circular punched out appearance. It is often painless, leading to a delay in presentation to a health professional. Tissue around the ulcer may become black, and gangrene may develop. Pedal pulses may be absent and reduced sensation can be demonstrated.
Diabetic foot ulcer
How Big Are Foot And Toe Ulcers
There are many different sizes of ulcers. They start as small as 1 centimeter wide and can grow to the size of your entire foot if left untreated.
The depth of the ulcer can change, too. Several different classification systems exist to define the depth of an ulcer. The Wagner Diabetic Foot Ulcer Grade Classification System, for example, has six grades:
- Grade 0: Your skin is intact .
- Grade 1: The ulcer is superficial, which means that the skin is broken but the wound is shallow .
- Grade 2: The ulcer is a deep wound.
- Grade 3: Part of the bone in your foot is visible.
- Grade 4: The forefront of your foot has gangrene .
- Grade 5: The entire foot has gangrene.
Classification Of Diabetic Foot Ulcers
The results of the foot evaluation should aid in developing an appropriate management plan. If an ulcer is discovered, the description should include characteristics of the ulcer, including size, depth, appearance, and location. There are many classification systems used to depict ulcers that can aid in developing a standardized method of description. These classification systems are based on a variety of physical findings.
One of the most popular systems of classification is the Wagner Ulcer Classification System, which is based on wound depth and the extent of tissue necrosis . Several authors have noted a disadvantage of this system in that it only accounts for wound depth and appearance and does not consider the presence of ischemia or infection.,
The University of Texas system is another classification system that addresses ulcer depth and includes the presence of infection and ischemia . Wounds of increasing grade and stage are less likely to heal without vascular repair or amputation.
Read Also: Gastric Ulcer Treatment In Horses
How Can I Reduce My Risk Of Foot And Toe Ulcers
There are several things you can do to help reduce your risk of getting foot and toe ulcers. Sometimes, adopting these habits can even stop them from coming back. Try to:
- Manage your diabetes. If you have diabetes you should wear appropriate footwear and never walk barefoot.
- Examine your legs as well as the tops and bottoms of your feet and the areas between your toes every day. Look for any blisters, cuts, cracks, scratches or other sores. Also check for redness, increased warmth, ingrown toenails, corns and calluses. Use a mirror to view your leg or foot if necessary. If its difficult to see, ask a family member to look at the area for you. See a healthcare provider immediately if you notice any problems.
- Talk to your healthcare provider about ways you can stop smoking.
- Manage your blood pressure.
- Control your cholesterol and triglyceride levels by changing your diet. Limit salt in your diet.
- Care for your toenails frequently. Cut your toenails after bathing, when they are soft. Cut toenails straight across and smooth with a nail file. Take care of ingrown toenails.
Its Been Longer Than Four Weeks
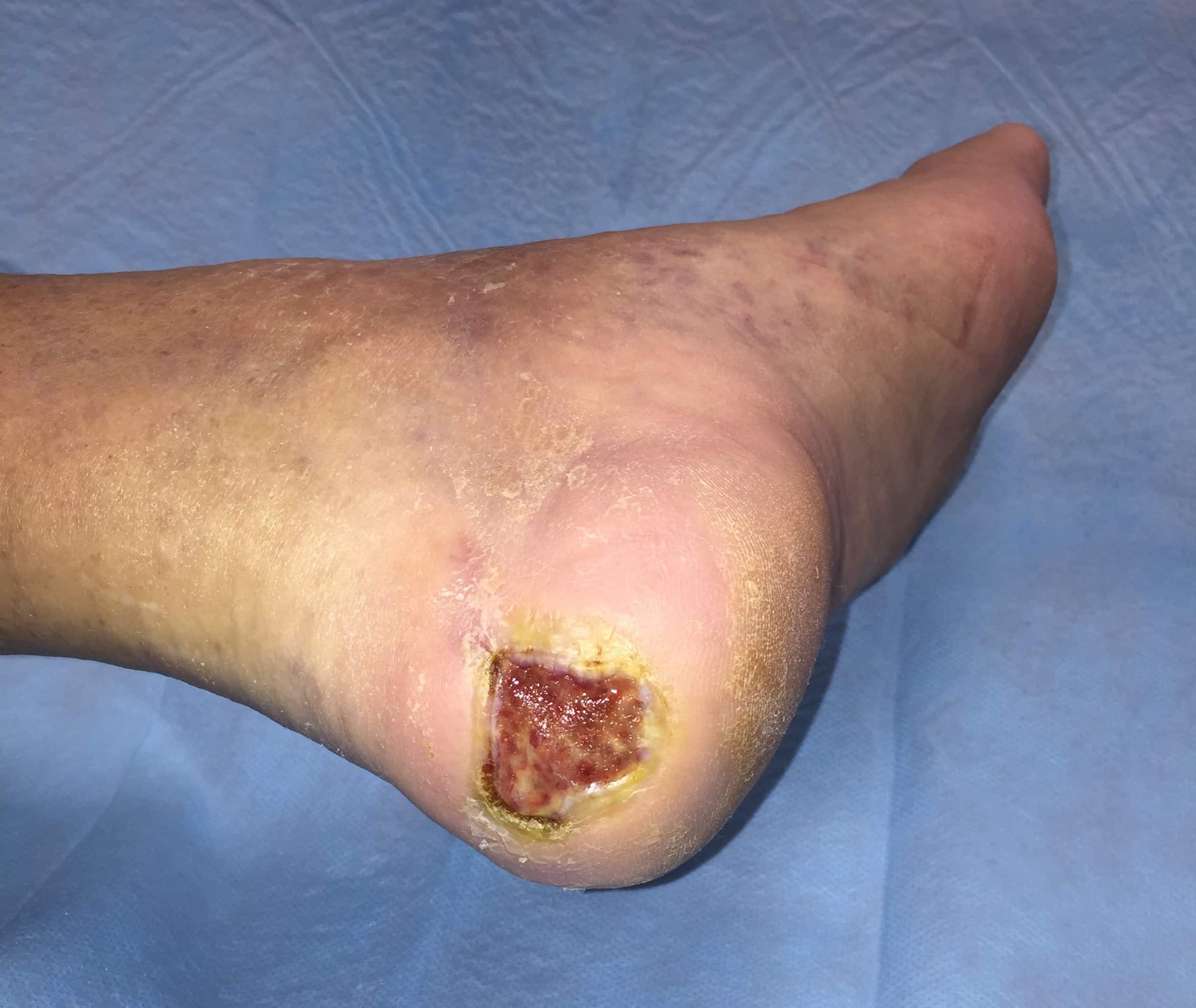
If wounds dont heal within a month, they are considered chronic wounds. While its possible for chronic wounds to heal on their own, its best to get a doctors help to identify why the wound isnt healing and provide treatment.
Our Wound Healing Center offers advanced treatments for severe and chronic diabetic wounds
You May Like: Symptoms Of Crohn’s And Ulcerative Colitis
What Is A Diabetic Foot Ulcer
A diabetic foot ulcer is an open sore or wound that occurs in approximately 15 percent of patients with diabetes and is commonly located on the bottom of the foot. Of those who develop a foot ulcer, 6 percent will be hospitalized due to infection or other ulcer-related complication.
Diabetes is the leading cause of non-traumatic lower extremity amputations in the United States, and approximately 14-24 percent of patients with diabetes who develop a foot ulcer will require an amputation. Foot ulceration precedes 85 percent of diabetes-related amputations. Research has shown, however, that development of a foot ulcer is preventable.
Diabetic Foot Ulcers Are Serious But Preventable
Ulcers are a warning sign from your feet worth paying attention to. According to Healthline, diabetic foot ulcers can be identified by symptoms such as pain, drainage, swelling, redness, and discolored tissue. These lesions are caused by poor circulation, nerve damage, and hyperglycemia — complications of unmanaged diabetes. However, anyone with diabetes can develop foot ulcers.
Diabetic foot ulcers may take weeks or even months to heal, per MedlinePlus. Treatment often involves removing dead skin and tissue around the ulcer and may require hospitalization. It’s also important to take care of the affected foot by wearing special shoes and using crutches or a wheelchair to avoid putting pressure on the ulcer.
If ulcers aren’t treated, they may lead to amputation. In fact, the University of Michigan Health estimates that between 14% and 24% of patients with diabetes who develop a foot ulcer will require amputation.
Proper treatment and prevention are key to avoiding these risks. People with diabetes should contact a medical professional immediately if they notice signs of an ulcer on the foot. Some people who are especially at risk — such as those with neuropathy, poor circulation, or uncontrolled blood sugar — should visit a podiatrist regularly to prevent ulcers from forming.
Recommended Reading: How Do I Tell If I Have An Ulcer
How Do I Take Care Of My Foot And Toe Ulcers
Your healthcare provider might teach you how to care for your ulcers at home. You might be instructed to:
- Wash the affected area with mild soap.
- Keep the wound clean and dry.
- Change the bandages as directed.
- Take prescribed medications as directed.
- Drink plenty of fluids. Ask your healthcare provider how much water you should drink every day.
- Follow a healthy diet, as recommended by your healthcare provider.
- Exercise regularly, under your healthcare providers care.
- Wear appropriate shoes.
- Wear compression wraps as directed.
Diabetic Foot Ulcers Or Wounds
If foot wounds are left untreated, they may turn into foot ulcers, which are often called diabetic foot sores. In its earliest stages, a diabetic sore may look like a blister or burn. About 20-25% of people with diabetes will get a foot ulcer at some point in their life.
Heres what causes diabetic foot ulcers
Most foot ulcers are on the ball of your foot, often near your big toe. A foot ulcer looks like a red sore. You may have an early-stage foot ulcer if drainage from the sore is clear. If theres colored pus and the wound smells badly, it may be infected.
If you have a foot ulcer, you should talk to your doctor about diabetic foot ulcer treatments. If its infected, you should make an appointment with your primary care doctor as soon as possible.
Foot ulcers can take a long time to heal about three months and youll need to check in frequently with a doctor to make sure that the healing process stays on track. In some cases, you may need special shoes to reduce pressure on the wound.
While this may all seem like a lot of work, theres a reason to stick with it. If your foot ulcer doesnt heal, it can turn into something more serious, possibly even the loss of a limb.
Read Also: Best Treatment For Diabetic Foot Ulcer
Find And Treat Cuts Scrapes And Other Wounds Immediately
If you treat new wounds right away, you can start caring for them before things get bad. So as soon as you find a cut or sore:
Of course, if you dont know you have a wound, you cant treat it quickly. So if you suffer from neuropathy, keep an eye out for new wounds. Check your hands and feet daily, and dont forget to check between your toes.
Wearing white socks can help, too. If you see a red spot or a place where your sock is sticking to your skin, check your foot to see if you have a wound thats new or not healing.
How Are Foot And Toe Ulcers Treated
The treatment of all ulcers begins with careful skin and foot care. Inspecting your skin is very important, especially for people with diabetes. Detecting and treating foot and toe sores early can help you prevent infection and keep the sore from getting worse.
The goal of treating a foot or toe ulcer is to heal your wound and relieve any pain. Your treatment plan will be individualized based on what medical condition is causing your ulcers. If you cant correct the cause of your ulcer, its likely to come back after treatment.
There are both surgical and nonsurgical treatments for foot and toe ulcers. For early-stage foot and toe ulcers, nonsurgical treatments might work. More advanced ulcers especially ones that are infected might require surgery.
Nonsurgical treatments include:
- Topical wound care.
- Reconstructive surgery using skin grafts.
Read Also: What To Eat When You Have A Stomach Ulcer
What Happens When You Have Diabetic Foot Ulcers
Diabetes is much more than the result of drinking too much sugary soda. While diet can contribute to diabetes, the disease can also be related to genetics, ethnicity, and age . Regardless of the cause, there’s no known cure for diabetes, according to WebMD. However, people who are diagnosed with the condition can take steps to manage their symptoms.
Symptoms vary based on the type of diabetes. The Centers for Disease Control and Prevention explains that symptoms of type 1 diabetes can be severe and may appear over a short amount of time. By contrast, the signs of type 2 diabetes are often less obvious and may go undetected for years. In either case, common symptoms can include frequent urination, persistent thirst and hunger, blurry vision, fatigue, weight loss, and sores or dry skin. People with diabetes may also notice they experience more infections than usual.
Additionally, diabetes can lead to a lesser-known but potentially dangerous symptom: foot ulcers. According to the University of Michigan Health, around 15% of people with diabetes will develop ulcers on their feet. If left untreated, these sores can result in serious complications.
What Are Neurotrophic Ulcers
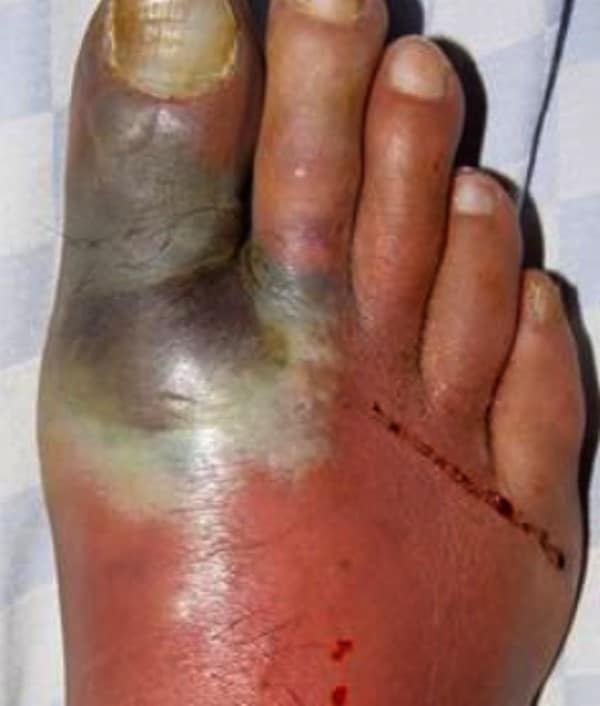
Neurotrophic ulcers occur primarily in people with diabetes, although they can affect anyone who has impaired sensation in their feet. They can be found anywhere on your feet, but they usually develop on the parts of your feet and toes that are most sensitive to weight .
Neurotrophic ulcers dont cause pain. But they can be serious if they arent treated promptly or they dont respond to treatment.
A neurotrophic ulcer might be the following colors:
- Any combination of those colors.
The thin borders of the ulcers are punched out, meaning that theyre taller than the surrounding tissues.
You May Like: How Do You Test For Stomach Ulcers
Who Gets Foot And Toe Ulcers
Foot and toe ulcers can happen to many people but might be more common in Black, Native American and Hispanic people. If you have an eye, kidney or heart disease related to diabetes, youre also at a higher risk. About 15% of people with diabetes will get an ulcer, typically on the bottom of their foot. Some of those people will be hospitalized because of complications.
Youre also at a higher risk of getting foot and toe ulcers if you have any of the following conditions:
- Blood circulation issues.
If your ulcer is black, that means cells in the tissues have died. This is called necrosis .
Foot Selfies May Improve Remote Diabetic Foot Monitoring
Nov. 12, 2021 — âFoot Selfiesâ may represent a simple solution to keeping tabs on patients who are at high risk for diabetic foot complications.
Patients with foot ulcers– or who are at risk for them– are told to check their feet regularly at home but doing so can be difficult for individuals who arenât flexible or who have vision problems. Those who live alone may not be able to ask someone else to check their feet for them. Some use hand mirrors, but those can be difficult to manipulate and donât offer feedback.
To address this problem, Mark Swerdlow, now a fourth-year medical student at the University of Southern California, Keck School of Medicine, Los Angeles, built a simple 3D-print device that allows patients to take standardized photos of the entire bottom surface of their own feet using a phone app with voice commands.
This âFoot Selfie Systemâ eliminates the need for assistance and allows the images to be sent to a clinician.
Swerdlow gave a live demonstration of the device during the recent virtual meeting of the Diabetes Technology Society. Results from a feasibility study of 15 patients were also online Oct. 31 in the Journal of Diabetes Science and Technology.
âThe point of it is to be a very simple tool that essentially anybody can use,â Swerdlow says.
Meanwhile, when asked to comment, Jan S. Ulbrecht, MD, called it âa very good idea.â
Patients Used the Device and Liked It
In the Meantime, just get Patients to take Pics of Their Feet
Read Also: Quantitative Research On Pressure Ulcer Prevention
Assessment Of Diabetic Foot Ulcers
A task force of the Foot Care Interest Group of the American Diabetes Association released a 2008 report that specifies recommended components of foot examinations for patients with diabetes. Providers should take a history that takes into consideration previous ulceration or amputation. The history should also include any neuropathic symptoms or symptoms that are suggestive of peripheral vascular disease. Further, providers should inquire about other complications of diabetes, including vision impairment suggestive of retinopathy and nephropathy, especially dialysis or renal transplantation. Finally, patients should be questioned regarding smoking because smoking is linked to the development of neuropathic and vascular disease. A complete history will aid in assessing the risk for foot ulceration.
In examining the foot, visual inspection of the bare foot should be performed in a well-lit room. The examination should include an assessment of the shoes inappropriate footwear can be a contributing factor to the development of foot ulceration. In the visual inspection of the foot, the evaluator should check between the toes for the presence of ulceration or signs of infection. The presence of callus or nail abnormalities should be noted. Additionally, a temperature difference between feet is suggestive of vascular disease.
Dont Wait The Consequences Of Non
Its difficult for researchers to determine just how many people have waited, as well as how long they typically wait, before going to the doctor. One study found that ulcers that have been present for about a month and a half before the first doctor visit were less likely to heal than ulcers that were seen and treated sooner. As previously mentioned, non-healing foot ulcers are often a sign of PAD, because a non-healing sore on the foot, toe, or ankle can be a sign of a malfunctioning circulatory system. This is important to realize, because there are minimally invasive PAD treatments that can help. Doing nothing, however, or waiting too long to see if the sore will heal, or get your PAD treated, can increase your risk for more serious complications, such as chronic infection, gangrene, and even amputation.
Also Check: What To Take If You Have A Stomach Ulcer
Keep Your Wound Clean And Covered With The Right Dressings
Wounds heal best when they are clean and moist. So its important to get them clean and covered right away. If you have a new scrape or cut, a basic bandage and antibiotic cream should work just fine.
But if you have wounds that are infected, slow healing or more serious, make an appointment with a doctor to learn what the best wound care is for you. Your doctor will likely recommend different types of diabetic wound care dressings to protect the injury and promote healing.
Common types of dressings for diabetic wound care
- Foam dressings Extremely soft and absorbent, foam dressings are used for wounds that leak or ooze a lot. They also offer added cushioning which can help protect the wound against physical damage.
- Alginate dressing These types of dressings are primarily made from seaweed. They can hold up to twenty times their weight in moisture, making them a great choice for deep wounds and ones with discharge. Another advantage of alginate dressings is that they prevent the growth of new bacteria.
- Hydrogel dressings Hydrogel is a water-based gel designed to keep an area moist. If your wound is dry or covered in dead skin, your doctor may recommend a hydrogel dressing to provide moisture. This can help break down dead tissue and promote cell growth. These types of dressings usually arent used for infected wounds.
Inflammation That Lasts Too Long Or Comes Back
Inflammation is a normal part of the healing process. But after about a week, the redness and swelling around your wound should be gone. If it isnt, something is getting in the way of the healing process.
Also, you should only see inflammation at the beginning of wound healing. If inflammation reappears later in the healing process, it may signal an infection or other problem.
Read Also: Best Ulcer Supplement For Horses