Risk Assessment And Prevention Of Pressure Ulcers
About this Guideline
Define early interventions for pressure ulcer prevention, and to manage Stage I pressure ulcers.
This best practice guideline assists nurses who work in diverse practice settings to identify adults who are at risk of pressure ulcers. This guideline focuses its recommendations on:
- Practice Recommendations including assessment, planning, intervention and discharge/transfer of care
- Educational Recommendations for supporting the skills required for nurses working with adults at risk for pressure ulcers
- Organization & Policy Recommendations addressing the importance of a supportive practice environment as an enabling factor for providing high quality nursing care, which includes ongoing evaluation of guideline implementation.
Revised: 2011
Nancy Parslow RN, CETN, MClSc Wound Healing Team LeaderKaren Campbell RN, MScN, PhDChris Fraser HBSc, RDConnie Harris RN, ET, IIWCC, MScKathryn Kozell RN, BA, MScN, APN, CETNJanet Kuhnke RN, BA, BScN, MS, ET, PhDKimberly LeBlanc RN, BScN, MN, CETNSusan Mills Zorzes RN, BScN, MDE, CWOCN, CETNLinda Norton OTReg., MScCHLyndsay Orr PT, MCLSc Wound HealingFruan Tabamo RN, BPh, BTh, MCLScLaura Teague RN, MN, NP-AdultKevin Woo RN, PhD, GNC, FAPWCAFrederick Go, RN, MNBa Pham MSc, PhD Advisory Panel Member
Fran MacLeod, RN, MScN Team LeaderPatti Barton, RN, PHN, ETKaren Campbell, RN, MSN
F Grading The Evidence For Each Key Question
The strength of evidence for each KQ will be assessed by one researcher for each applicable outcome by using the approach described by Owens et al.10 To ensure consistency and validity of the evaluation, the grades of each reviewer will be reviewed by the entire team of investigators to evaluate:
- Risk of bias
- Consistency
- Directness
- Precision
We will also estimate publication bias by examining whether studies with smaller sample sizes tended to have positive or negative assessments of pressure ulcer treatment.
The strength of evidence will be assigned an overall grade of high, moderate, low, or insufficient according to a four-level scale:
- HighâHigh confidence that the evidence reflects the true effect. Further research is very unlikely to change our confidence in the estimate of effect.
- ModerateâModerate confidence that the evidence reflects the true effect. Further research may change our confidence in the estimate of effect and may change the estimate.
- LowâLow confidence that the evidence reflects the true effect. Further research is likely to change the confidence in the estimate of effect and is likely to change the estimate.
- InsufficientâEvidence either is unavailable or does not permit estimation of an effect.
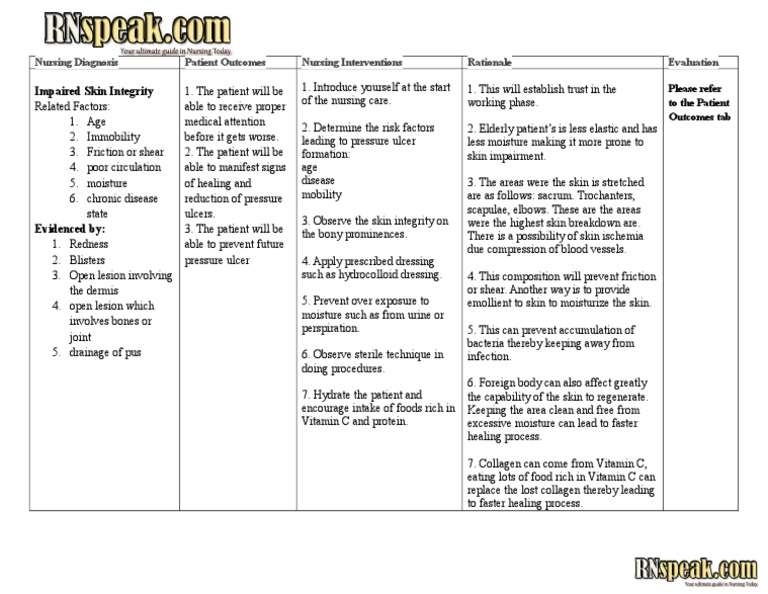
Pressure Ulcer Nursing Care Plans Diagnosis And Interventions
Pressure Ulcer NCLEX Review and Nursing Care Plans
Pressure ulcers, sometimes called bedsores or Decubitus ulcers, are skin and tissue breakdown that arises from exertion of incessant pressure to the skin. Continuous stress to the skins integrity will eventually cause skin breakdowns.
The development of pressure ulcers is an example of such skin damage. The most common sites of injuries are the bony prominences of the body, such as the heels, knees, elbows, and sacrum.
There are different stages of pressure ulcers in terms of severity. Not all stages of pressure ulcers present with open sores. The National Pressure Injury Advisory Panel has coined that the most appropriate term should be pressure injuries.
Problems on mobility, poor nutrition, among others, predispose patients in having this condition.
Also Check: How Long Does An Ulcerative Colitis Flare Up Last
Protecting Fragile Skin: Nursing Interventions To Decrease Development Of Pressure Ulcers In Pediatric Intensive Care
Christine A. Schindler Theresa A. Mikhailov Evelyn M. Kuhn Jean Christopher Pat Conway Debra Ridling Annette M. Scott Vickie S. Simpson Christine A. Schindler Theresa A. Mikhailov Evelyn M. Kuhn Jean Christopher Pat Conway Debra Ridling Annette M. Scott Vickie S. Simpson Christine A. Schindler Theresa A. Mikhailov Evelyn M. Kuhn Jean Christopher Pat Conway Debra Ridling Annette M. Scott Vickie S. Simpson Christine A. Schindler Theresa A. Mikhailov Evelyn M. Kuhn Jean Christopher Pat Conway Debra Ridling Annette M. Scott Vickie S. Simpson Christine A. Schindler Theresa A. Mikhailov Evelyn M. Kuhn Jean Christopher Pat Conway Debra Ridling Annette M. Scott Vickie S. Simpson Christine A. Schindler Theresa A. Mikhailov Evelyn M. Kuhn Jean Christopher Pat Conway Debra Ridling Annette M. Scott Vickie S. Simpson Christine A. Schindler Theresa A. Mikhailov Evelyn M. Kuhn Jean Christopher Pat Conway Debra Ridling Annette M. Scott Vickie S. Simpson Christine A. Schindler Theresa A. Mikhailov Evelyn M. Kuhn Jean Christopher Pat Conway Debra Ridling Annette M. Scott Vickie S. Simpson
Christine A. Schindler, Theresa A. Mikhailov, Evelyn M. Kuhn, Jean Christopher, Pat Conway, Debra Ridling, Annette M. Scott, Vickie S. Simpson Protecting Fragile Skin: Nursing Interventions to Decrease Development of Pressure Ulcers in Pediatric Intensive Care. Am J Crit Care 1 January 2011 20 : 2635. doi:
Purpose Of Systematic Review

Knowledge is translated from research into clinical practice based on the evidence reported by systematic reviews . Yet, there has not been a systematic review of the intensive care literature published since 2002 for HAPU prevention strategies incorporating the Braden scale , and none focused on care bundles. The purpose of this systematic review was to evaluate the effectiveness of care bundles incorporating the Braden scale for risk assessment in reducing the HAPU prevalence in older adults hospitalized in the ICU.
Recommended Reading: Crohns Versus Ulcerative Colitis Pathology
You May Like: Cost Of Biologics For Ulcerative Colitis
What Are The Best Practices In Pressure Ulcer Prevention That We Want To Use
Once you have determined that you are ready for change, the Implementation Team and Unit-Based Teams should demonstrate a clear understanding of where they are headed in terms of implementing best practices. People involved in the quality improvement effort need to agree on what it is that they are trying to do. Consensus should be reached on the following questions:
In addressing these questions, this section provides a concise review of the practice, emphasizes why it is important, discusses challenges in implementation, and provides helpful hints for improving practice. Further information regarding the organization of care needed to implement these best practices is provided in Chapter 4 and additional clinical details are in Tools and Resources.
In describing best practices for pressure ulcer prevention, it is necessary to recognize at the outset that implementing these best practices at the bedside is an extremely complex task. Some of the factors that make pressure ulcer prevention so difficult include:
You May Like: How To Stop An Ulcerative Colitis Flare
Treatment For Pressure Ulcers
The ulcers are treated with methods that promote wound healing and prevent further damage, such as
-Preventing deep or prolonged contact with a hard surface. This is done by using a unique cushion called an air body or air mattress. This helps maintain position, prevent shearing and improve circulation to the wound site.
-Removing or repositioning any objects in contact with the ulcer, such as clothing or sheets.
-Lifting extremities for bedridden patients. A unique tool called the McRoberts maneuver can raise a leg while the patient is lying on their back. This will help prevent pressure from being placed on that area and allow it to heal.
-Turning/repositioning bed-bound patients every two hours if possible. If not, reposition as often as possible for the patient.
-Prompt treatment of any skin breakdown with a topical or local wound-care product that will protect the skin from further damage.
Recommended Reading: Corneal Ulcer Dog Home Remedy
Ethics Approval And Consent To Participate
Initially ethical clearance was obtained from Addis Ababa University, College of Health Sciences, Department of Nursing and Midwifery Research Review Ethical Committee, and Addis Ababa Regional Health Bureau Ethical Clearance Committee for four hospitals includedin the study to obtain participants in each hospitals. The sixth hospital is teaching hospital administered by Addis Ababa University. These findings were part of a research titled An assessment Nurses knowledge, attitude and practice towards pressure ulcer prevention in admitted patients in Public referral hospitals in Addis Ababa. Permissions to obtain participants secured from each hospital medical directors, matrons and head nurses for the research to be undertaken at each hospital. The anonymity of the participants was respected. The names of the participants were not mentioned to keep the confidentiality. A signed written consent was obtained from participants before participation.
What Causes Pressure Ulcers
-Pressure ulcers often develop with prolonged pressure on the skin. This may be due to sitting in a chair or lying down for long periods without repositioning. It can also occur if someone is seated or lying in one position and their weight shifts to one side, applying pressure on just one area of the body.
Poor nutrition, dehydration, and lack of mobility are common factors in developing pressure ulcers.
-Pressure ulcers are also more likely to develop in people who wear restrictive clothing, including tight-fitting pants, belts, or collars. The pressure from these garments can cause injury even without weight being applied directly to the affected area.
You May Like: Best Foods To Eat With A Peptic Ulcer
Causes And Risk Factors Of Pressure Ulcer
Pressure ulcers are caused by relentless pressure against the skin, thereby limiting blood flow to the skin and its surrounding tissues.
Inactivity and limited movement, particularly on bed-ridden patients, makes the skin vulnerable for the development of pressure ulcers.
There are three contributing factors for its development, and they are:
The risk factors of pressure ulcers are the following:
Skin Integrity Nursing Care Plans
-Provide the patient with a scheduled play, pain management, and device change.
-Upon noticing the presence of redness or changes in skin temperature, notify the charge nurse immediately. This is to prevent further breakdown and eliminate serious complications such as infection.
-Adjust bed height or reposition the patient to prevent further pressure on the area.
-Assess precautions/contraindications: Review updated physician orders, laboratory and diagnostic studies, and current medication.
-Identify and eliminate/minimize the risk of exposure: Use standard precautions as appropriate for all patients, including transmission-based precautions when indicated.
Protect exposed areas from further damage: Use protective devices such as skin barriers or glove powder to reduce friction during patient repositioning and transfers.
-Instruct patient/family of home care to include:
Daily inspection for proper wound dressing and possible signs or symptoms of infection.
Change bandages as needed to maintain the integrity of the skin edges.
Keep wound area clean and dry. Use hydrogel dressings as ordered and according to the manufacturers recommendation.
Educate on the need to provide adequate nutrition and enough fluids for hydration to the patient.
We also have care plans for Cellulitis
Get the following premium features for free after ordering a custom nursing assignment from us:
- Formatting
Monitor the patients skin daily to ensure proper hygiene.
Don’t Miss: How Does Ulcerative Colitis Affect The Body
Overall Theme: Prevention Of Pressure Ulcers Is Important In The Care Of Geriatric Patients
All the nurses interviewed stated that the topic of pressure ulcers was of essential importance in nursing care, in particular when caring for geriatric patients. It was expressed that skin care and observations hereof is considered as one of the fundamental nursing tasks in nursing geriatric patients.
During the interviews, four sub-themes emerged and all sub-themes were chosen according to how the nurses explained their experiences with perception and perception of pressure ulcers: Nursing resources on the ward, Basic nursing skillslift the duvet, Introduction of new nurses on the wardbedside teaching and Missing articulation of pressure ulcers.
B Searching For The Evidence: Literature Search Strategies For Identification Of Relevant Studies To Answer The Key Questions
To identify primary literature, we will search the following databases: MEDLINE® , EMBASE® , CINAHL® , Evidence-Based Medicine Reviews , the Cochrane Central Register of Controlled Trials, the Cochrane Database of Systematic Reviews , the Database of Abstracts of Reviews of Effects , and the Health Technology Assessment Database. We will search broadly for pressure ulcer treatments with a date limit of 1985 to the present Table 1 shows a sample of the search strategy we will use. Grey literature will be identified by soliciting stakeholders, seeking recommendations from the TEP, and searching relevant Web sites including: clinical trial registries regulatory documents conference proceedings and dissertations , and Dissertations & Theses Database ), and individual product Web sites. Additional studies will be identified by reviewing the reference lists of published clinical trials and review articles.
| 1 | |
|---|---|
| limit 4 to yr=”1985 -Current” | |
| 6 | remove duplicates from 5 |
Scientific information packets will be requested from identified manufacturers. Other drug or device manufacturers not identified in the SIP requisition process will have the opportunity to submit data for this review by using the online SIP portal on the AHRQ Effective Health Care Program Web site. Reviewers will evaluate the SIPs we receive for data relevant to our review.
Read Also: Can I Take Tylenol With An Ulcer
Staging Of Pressure Injuries: Based On National Pressure Injury Staging System
Stage 1: Skin is completely intact! The area will be very red but it does NOT blanch .
Stage 2: Skin is visibly damaged and NOT intact with PARTIAL loss of the dermis. No subq will be visible. Wound may be opened with superficial red/pink opened ulcer or may have the formation of an opened or closed blister.
Stage 3: Skin is visibly damaged and NOT intact with FULL loss of the skin tissue. May see the subq . Wound edges may be rolled away..epibole. Bone, tendon and muscle NOT visible.
Stage 4: Skin is visibly damaged with FULL loss of the skin tissue that will expose bone, muscle, tendon, and ligaments.
Unstageable:
Slough or eschar is covering a full thickness ulcer. You cant assess the actual depth of the wound because of the slough or eschar covering the ulcer.
Deep-Tissue Injury:
Presents as purplish or blackish areas over skin that is intact. The fatty tissue below is injured. Also, may look like a black blister area. It may feel heavy or spongy.
Background And Objectives For The Systematic Review
Uninterrupted pressure exerted on the skin, soft tissue, muscle, and bone can lead to the development of localized ischemia, tissue inflammation, tissue anoxia, and necrosis. Pressure ulcers can result from these effects about 3 million adults in the United States suffer from pressure ulcers. Estimates of the incidence of pressure ulcers vary according to the setting and range from 0.4 to 38.0 percent in acute-care hospitals, from 2.2 to 23.9 percent in long-term nursing facilities, and from 0 to 17 percent in the home-care setting.1,2 Various systems have been used to assess the severity of pressure ulcers, but most use a four-stage categorization with higher numbers indicating higher severity.3 Healing rates of pressure ulcers vary considerably and are dependent on comorbidities, clinical interventions, and severity of the ulcer. This variability can add to the length of hospitalization and impede the return of patients to full functioning.2 Data on the costs of treatment for a pressure ulcer vary, but some estimates range between $37,800 and $70,000, with total annual costs in the United States as high as $11 billion.1,4
Read Also: What Should You Not Eat With An Ulcer
Classification Of Pressure Ulcers
Depending on various characteristics, pressure ulcers are classified under the International NPUAP- EPUAP Pressure Ulcer Classification System. Accordingly there are 4 grades from 1 to 4 and their characteristics are as follows:
GRADE 1: Non-blanchable erythema of intact skin Discolouration of the skin, warmth, oedema, induration or hardness can also be used as indicators, particularly on individuals with darker skin.
GRADE 2: partial thickness skin loss involving epidermis or dermis, or both. The ulcer is superficial and presents clinically as an abrasion or blister.
GRADE 3: full thickness skin loss involving damage to or necrosis of subcutaneous tissue that may extend down to, but not through, underlying fascia
GRADE 4: extensive destruction, tissue necrosis, or damage to muscle, bone or supporting structures with/without full thickness skin loss.
Pressure ulcer grade should be recorded using the EPUAP classification system and all pressure ulcers graded 2 and above should be documented as a local clinical incident.
The Nurses Advocacy Role
Falls and pressure ulcers in elderly patients are nothing new, but these never events are getting more attention. They also have potential legal ramifications: A pressure ulcer that develops during a patients hospital stay may be grounds for a professional liability lawsuit. Hospitals may suffer financially because their reimbursements may decrease if safety measures arent carried out properly.
Acting as a patient advocate from admission through discharge can help you keep your patients safe. Advocate for hospital policies that help ensure patients stay safe. For instance, policies for fall-risk assessment programs with comprehensive guidelines for reducing and preventing falls can be created and implemented through fall-prevention teams and quality-improvement or risk-management teams.
Of course, nurses alone arent responsible for patient safety. All hospital employees must make patient safety a goal, including housekeeping, food services staff, certified nurse aides, and administrators. We often criticize patients for being nonadherent when the real problem may be lack of available services or inability to access them. Such services include a home hazards assessment, implementation of a fall-proofing plan, an at-home exercise program, and installation of a fall-proof alert system. Preventing falls both in the hospital and at home and increasing your knowledge of pressure ulcer prevention and management can help you keep patients in good health.
Selected references
Recommended Reading: Early Symptoms Of Ulcerative Colitis