What Are The Causes Of Ulcerative Colitis
The exact cause of ulcerative colitis is unknown. The following have been suggested:
- Immune system
- Ulcerative colitis is thought to be a type of autoimmune disease, in which the body’s immune system malfunctions and attacks the tissues of the bowel.
Ulcerative colitis may occur at any age, but it is most common in young adults in the 15-30 age group or later on, in the 50-70 age group. Women are affected more than men.
What Should I Ask My Doctor On Behalf Of My Child Or Teenager
Ask your healthcare provider the following questions in addition to the ones listed above:
- What vitamins should my child take?
- Will my other children have pediatric ulcerative colitis?
- Is my child at risk for other conditions?
- Can you recommend a psychiatrist or therapist to help my child with emotional issues related to pediatric ulcerative colitis?
- Is my child growing at a normal rate?
- What can I do to help my child cope at school?
A note from Cleveland Clinic
When you have ulcerative colitis, its essential to work closely with your healthcare team.
Take your medications as prescribed, even when you dont have symptoms. Skipping medications youre supposed to take can lead to flareups and make the disease harder to control. Your best shot at managing ulcerative colitis is to follow your treatment plan and talk to your healthcare provider regularly.
What Is Ulcerative Colitis
Ulcerative colitis causes irritation and ulcers in the large intestine . It belongs to a group of conditions called inflammatory bowel disease . It often causes diarrhea with blood, cramping and urgency. Sometimes these symptoms can wake a person up at night to go to the bathroom as well.
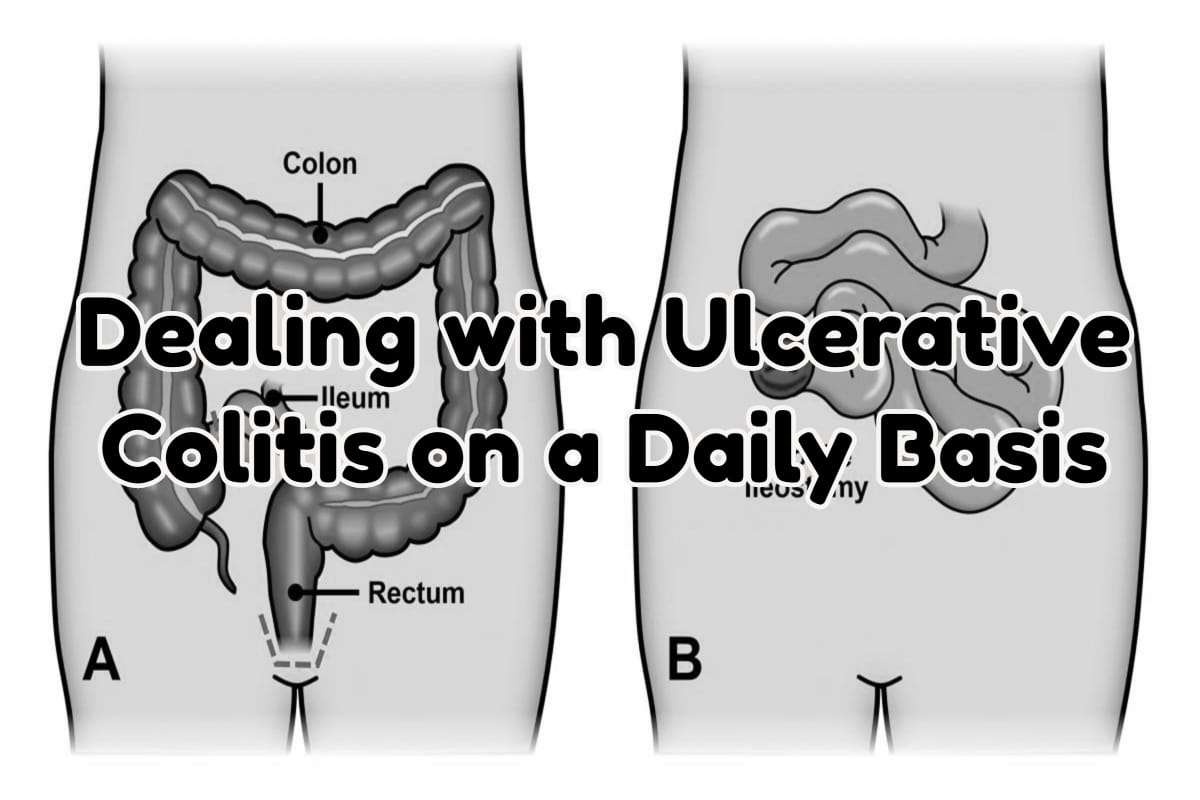
The inflammation in ulcerative colitis usually starts in the rectum, which is close to the anus . The inflammation can spread and affect a portion of, or the entire colon. When the inflammation occurs in the rectum and lower part of the colon it is called ulcerative proctitis. If the entire colon is affected it is called pancolitis. If only the left side of the colon is affected it is called limited or distal colitis.
The severity of UC depends on the amount of inflammation and the location. Everyone is a little different. You could have severe inflammation in the rectum or very mild inflammation in the entire colon .
If you have ulcerative colitis, you may notice a pattern of flare-ups , when symptoms are worse. During times of remission, you might have little to no symptoms. The goal with therapy is to remain in remission as long as possible .
You May Like: Can You Get An Ulcer In Your Intestines
How Is Ulcerative Colitis Diagnosed
To diagnose ulcerative colitis in children, teenagers and adults, your healthcare provider has to rule out other illnesses. After a physical exam, your provider may order:
- Blood tests: Your blood can show signs of infection or anemia. Anemia is a low level of iron in your blood. It can mean you have bleeding in the colon or rectum.
- Stool samples: Signs of infection, parasites , and inflammation can show up in your poop.
- Imaging tests: Your healthcare provider may need a picture of your colon and rectum. You may have tests including a magnetic resonance imaging scan or computed tomography scan.
- Endoscopic tests: An endoscope is a thin, flexible tube with a tiny camera. Specialized doctors can slide the endoscope in through the anus to check the health of the rectum and colon. Common endoscopic tests include colonoscopy and sigmoidoscopy.
What Are The Symptoms Of Ulcerative Colitis
Ulcerative colitis symptoms often get worse over time. In the beginning, you may notice:
- Diarrhea or urgent bowel movements.
- Abdominal cramping.
- Liver disease.
- Loss of fluids and nutrients.
Symptoms are similar in pediatric ulcerative colitis and may also include delayed or poor growth. Some ulcerative colitis symptoms in children can mimic other conditions, so it is important to report all symptoms to your pediatrician.
Recommended Reading: How To Treat Sacral Pressure Ulcer
How Long Do Flares Last
Flares occur at different times and may last for days or weeks. They can happen anywhere from weeks to years apart, depending on the person and the effectiveness of treatment.
Your doctor will work with you to treat your flare and help return your UC to a more manageable state.
The Crohns & Colitis Foundation recommends waiting to become pregnant until UC has been in remission for at least 3 months.
If you conceive during a flare-up, you may have more symptoms during pregnancy.
Youre likely to have a healthy pregnancy if you have UC, but youll still have a higher chance of complications than someone without the condition. Particularly if your UC is active, you may have a greater risk for:
- miscarriage
In general, UC medications can be taken during pregnancy.
Talk with your doctor about any possible changes to your medications while pregnant.
Ideally, having a conversation with your doctor prior to getting pregnant can allow them to prepare a UC treatment plan in advance that can be revised, if and as needed, during your pregnancy.
Get Ahead Of Your Stress
Megan Starshak, 36, has been dealing with ulcerative colitis since 2002, getting regular IV infusions of a biologic to keep her symptoms under control. But she’s well aware there will sometimes be bad days where she may have up to five bowel movements. “After a super stressful day, I’ll notice that I have more pain and looser stools,” she says.
Once, before an important presentation, she got incredibly sick and found herself wondering if she should go to the presentation or the hospital. Fortunately, a friend stepped in, telling her, “Whatever happens, your life is going to go forward”and that her health was more important than her work obligation. “Thats a moment I’ve kept with me,” she says. “Ive learned to let go of things that really dont matter in the long run.”
Starshak says she now tries to plan better when she knows there’s a stressful week ahead. “Don’t wait until youre in the middle of it to recognize your stress is high,” she says. “Getting ahead of it is crucial.” She recommends any version of stress management that works for you, such as yoga or taking a walk.
Read Also: Why Do You Get Mouth Ulcers
Will Ulcerative Colitis Affect Me Over Time
The effects of ulcerative colitis vary considerably from person to person, based on the nature and severity of their disease. In many cases, the condition does not have much impact on daily life, the ability to work or to enjoy an active social life but does take some getting used to. When it is at an active stage, symptoms such as diarrhoea and abdominal pain often require time away from work, college etc. and can make it difficult to cope going out or even being at home. However, treatment usually makes the symptoms better within days or weeks so normal quality of life can be restored quite quickly. Some severe cases of ulcerative colitis, however, can have a significant impact on peoples lives. This can be due to a weak response to treatment which makes symptom-free remission difficult to achieve and can involve frequent flare ups.
Failure To Have A Gastroenterology Specialist On Your Side
Your primary care physician can only do so much for you. In order to adequately manage and treat your Crohns or ulcerative colitis, you will need to see a specialist for regularevaluation. In fact, you should have a whole team of doctors working for you, from surgeons to radiologists to nutritionists however, your gastroenterologist should be your main point of contact when it comes to your condition.
We treat patients with Crohns and ulcerative colitis as well as a variety of other gastrointestinal diseases, including colon cancer, hepatitis, biliary diseases, esophageal disorders, and peptic ulcer disease. Our specialists can offer you more tips on how to best manage your condition, and work with you one-on- one to develop a workable treatment plan.
Please note, the information provided throughout this site is not intended or implied to be a substitute for professional medical advice, diagnosis or treatment. All content, including text, graphics, images, and video, on or available through this website is for general information purposes only. If you are experiencing related symptoms, please visit your doctor or call 9-1-1 in an emergency.
GET OUR FREE NEWSLETTER
You May Like: What Should You Not Eat With An Ulcer
Also Check: How To Prevent Skin Ulcers
How Long Do Flare
UC is a condition that is unique to every individual. Some people experience flare-ups that last a few days, while others experience flare-ups that last weeks. Likewise, individuals may go from a mild flare-up to a severe one and then back again.
If a person is experiencing a severe flare-up that persists, they should speak with a doctor. The doctor will help them get their symptoms under control and improve their quality of life.
How To Treat Ulcerative Colitis Naturally At Home 10 Tips
Ulcerative colitis is an inflammatory bowel condition that can cause the inflammation of the rectum and colon. It is known as an autoimmune disease in which the immune system attacks the healthy tissues inside the body, leading it to turn into inflamed.
There is still no research that confirms the exact reason for this disease. It is believed that a combination of environmental and genetic factors contribute to this health issue. Stress can even worsen the symptoms of this disease.
Ulcerative colitis can make the symptoms such as abdominal discomfort or pain, rectal bleeding, diarrhea, and production of pus caused by the ulcers or sores in the large intestine inner lining. The signs of this disease often go after coming, but 5 10 % of patients dealing with this condition face the symptoms of the disease all the time.
Also Check: Pressure Ulcers Are Most Likely To Develop
Scope Out The Menu Ahead Of Time
Mary Elizabeth U., 34, was diagnosed with ulcerative colitis 10 years ago after having a lot of diarrhea, cramping, and weight loss. Although Mary Elizabeth takes a biologic medication to manage her symptoms, she knows that some food and drinks will likely cause cramps and diarrhea for herfried foods, broccoli, cauliflower, and alcohol, specifically. Mary Elizabeth always tries to do a little digging about the menu so she can prepare ahead of time whenever her plans include food. She also regularly carries snacks with her just in case there are surprises on the food front.
If Im going to a wedding, I will talk to the bride or groom to see what theyre going to have. If I go to a restaurant, Ill look up the menu ahead of time, she tells SELF. If there isnt food I can have, Ill bring something of my own or eat before I go.
Can I Get Surgery For My Ulcerative Colitis

Surgery is an option if medications arent working or you have complications, such as bleeding or abnormal growths. You might develop precancerous lesions, or growths that can turn into colorectal cancer. A doctor can remove these lesions with surgery or during a colonoscopy.
Research shows that about 30% of people with ulcerative colitis need surgery sometime during their life. About 20% of children with ulcerative colitis will need surgery during their childhood years.
There are two kinds of surgery for ulcerative colitis:
Proctocolectomy and ileoanal pouch
The proctocolectomy and ileoanal pouch is the most common procedure for ulcerative colitis. This procedure typically requires more than one surgery, and there are several ways to do it. First, your surgeon does a proctocolectomy a procedure that removes your colon and rectum. Then the surgeon forms an ileoanal pouch to create a new rectum. While your body and newly made pouch is healing, your surgeon may perform a temporary ileostomy at the same time. This creates an opening in your lower belly. Your small intestines attach to the stoma, which looks like a small piece of pink skin on your belly.
After you heal, waste from your small intestines comes out through the stoma and into an attached bag called an ostomy bag. The small bag lies flat on the outside of your body, below your beltline. Youll need to wear the bag at all times to collect waste. Youll have to change the bag frequently throughout the day.
Also Check: How Do They Treat Stomach Ulcers
Know What To Watch For
You know your body best. But talk to your doctor about what a flare might look like for you. If you have mild symptoms, it might be OK to watch and wait for a day or so.
Signs to look for include:
- Blood in your stool
- Urgent need to empty your bowel
- Belly cramps
- A feeling that you canât empty your bowel
- Mouth sores
- Rashes or other skin problems
- Joint pain
Ask your doctor which symptoms signal an emergency. Let them know right away if you have:
- High fever
- Pain that doesnât go away
- Constant diarrhea or throwing up
- Lots of blood in your stool
Use Prescription Medication For Painful Flare Ups
I rely on natural remedies to prevent my symptoms of ulcerative colitis from flaring, and I use prescription medication to ease the painful symptoms when my colitis actually flares. Ive learned how to recognize when my guts are gearing up to explode, and I try to head it off at the pass. How do I know when the colitis is about to flare? The very bottom of my rectum starts to feel swollen and slightly uncomfortable. I can literally feel it starting to swell! So I use an enema before bed Id rather prevent a flare than spend time trying to ease the pain of my ulcerative colitis symptoms.
Pentasa enemas work best for me. Ive tried all sorts of suppositories, oral medications, and enemas to ease the painful symptoms of ulcerative colitis. A liquid enema is my best friend before and during a flare up. Enemas are more effective than suppositories because the liquid soaks into the bowel quickly and easily. I used suppositories for eight years after I was diagnosed with colitis, until a new gastroenterologist recommended enemas instead.
While I wish my first way to keep my ulcerative colitis in remission wasnt with prescription medication, I havent found anything else that works as good as the drugs. It doesnt matter what I eat I can eat popcorn, nuts, caffeine, dairy but when my colitis wants to flare, the only thing that tamps it down is an enema.
Recommended Reading: Home Remedies For Dog Mouth Ulcers
Spend More Time In Delta Sleep
Sleep keeps my colitis in remission. When I travel, get jet lag, or even stay out past midnight, I know Im setting myself up for a painful flare up. So I always say that one of the best ways to keep ulcerative colitis or any inflammatory bowel disease in remission is to sleep, sleep, SLEEP. I get eight hours a night, and often take a 30 minute nap during the day. I also try to get at least three hours of sleep before midnight. Ive found that getting eight hours of sleep after midnight doesnt make me feel as rested as sleeping before midnight does.
Sleep can keep the symptoms of ulcerative colitis in remission for so many reasons, both physical and emotional. Sleep helps restore brain and cell energy, recharges our minds and bodies, increases protein buildup, helps maintain social and emotional functioning, helps encode memories, improves learning ability, and helps process memories.
If you have trouble sleeping, read Natural Sleep Remedies for Sleepless Nights.
Crohns Disease And Ulcerative Colitis And Diet
Diet and food allergies do not cause IBD, and long-term special diets are not effective in treating IBD. However, adjusting your diet can help manage some of your symptoms, and can help IBD medications work better. A person with IBD has to pay close attention to their diet, since they may have malnutrition.
Recommended Reading: Will Ulcer Cause Back Pain
Keep An Emergency Kit On Hand
Megan says never knowing when a flare-up will start is one of the hardest aspects of managing ulcerative colitis. I might be feeling okay when I go out, but a bowel movement could hit at any time, she says. If I cant get to the bathroom quickly, Im going to have an accident and the whole night is going to turn around.
Thats why Megan keeps a clean-up kit handy, which was crucial in her early 20s when her symptoms were at their worst. Before I was in deep remission, Id always have a clean-up kit with me that had wipes, hand sanitizer, and underwear. Id keep a whole extra pair of pants in my car, she says. Just knowing that she has whatever she needs for a worst-case scenario makes her feel more confident about making plans.
Related:
Give Yourself Some Tlc
Stress doesn’t cause UC, but it makes symptoms and flares worse for some people. If it affects you, try meditation, breathing exercises, or a massage. You could also see a pro to try biofeedback, hypnotherapy, or a type of counseling called cognitive behavioral therapy, which helps you learn new ways to handle problems. Being active helps, too. Try yoga, tai chi, or other low-impact exercises like walking.
10
You May Like: How To Heal An Ulcer In The Esophagus