Interaction Between Stress And Ibd
In the 1950s, IBD was considered a psychosomatic disorder , and previous studies have demonstrated a close association between IBD and stress. Specifically, IBD patients are often exposed to stress, which induces mood swings or even leads to mental complications. Meanwhile, increased emotional disorders can exacerbate symptoms such as abdominal pain, and can enhance the severity of IBD in turn.
Fatigue In Children With Ulcerative Colitis
In a 2019 study , researchers looked at how children with ulcerative colitis experienced fatigue.
They found that, like adults, children with the condition can experience high levels of fatigue. They noted the following potential reasons for this:
- disease activity level
According to the Crohns and Colitis Foundation, fatigue is a common issue among people with IBD. It affects 80% of people with active IBD and 50% of people in clinical remission.
Despite the frequency of fatigue in IBD, researchers have indicated that it is often underreported and undertreated. They have noted that doctors often do not treat fatigue because of the subjective nature of the condition.
People with fatigue should talk with a doctor and make sure that they understand how much fatigue affects their life. The more information a person can provide about their symptoms, the more likely the doctor is to understand fatigue as a serious symptom and make recommendations for treatment.
In addition to taking steps to manage and treat ulcerative colitis, a person can make certain lifestyle changes to help reduce fatigue.
Some potential ways for a person to improve fatigue and boost energy levels include:
In one 2020 study , researchers found that the best way to treat fatigue is to treat its underlying causes.
Also Check: What To Take For Stomach Ulcer Pain
Can Stress Cause Uc
UC develops through interactions among genetics, environmental factors and gut . That part we have a handle on. The waxing and waning of the disease symptoms indicates there may be other factors at play including psychological stress. The jury is still out on whether stress can cause UC, but there are signals from the UC research community that an answer might not be too far in the distance.
For example, there is growing evidence from different studies suggesting that stress can act to promote relapses in inflammatory bowel disease according to the journal Frontiers in Pediatrics. There are also mice studies that show white blood cells are significantly increased after stress. Gut microbiota is also dramatically changed after stress, with more inflammation-promoting bacteria as reported in the journal Proceedings of the National Academy of Sciences. Researchers believe that the results of the mice studies show chronic stress disturbs gut microbiota, triggering immune system response and facilitating colitis. While there is still a lot to learn about whether stress can cause UC, there is one thing we know for sure: When we experience prolonged stress, multiple systems of our body are impacted and usually not in a good way.
You May Like: Colon Cleanse For Ulcerative Colitis
Try Hypnotherapy To Prolong Clinical Remission
Hypnotherapy uses guided meditation and concentration to achieve a heightened state of awareness. Gut-directed hypnotherapy can influence gut secretions, reduce pain, and prolong remission in those with UC, says Dr. Kinsinger.
A review published in June 2020 in The American Journal of Gastroenterology notes that while hypnotherapy may not relieve symptoms of UC, it may help improve your quality of life by reducing stress.
Go to a trained professional to receive hypnotherapy, says Lilani Perera, MD, a gastroenterologist with Advocate Aurora Health in Grafton, Wisconsin.
What Causes Ulcerative Colitis Flareups
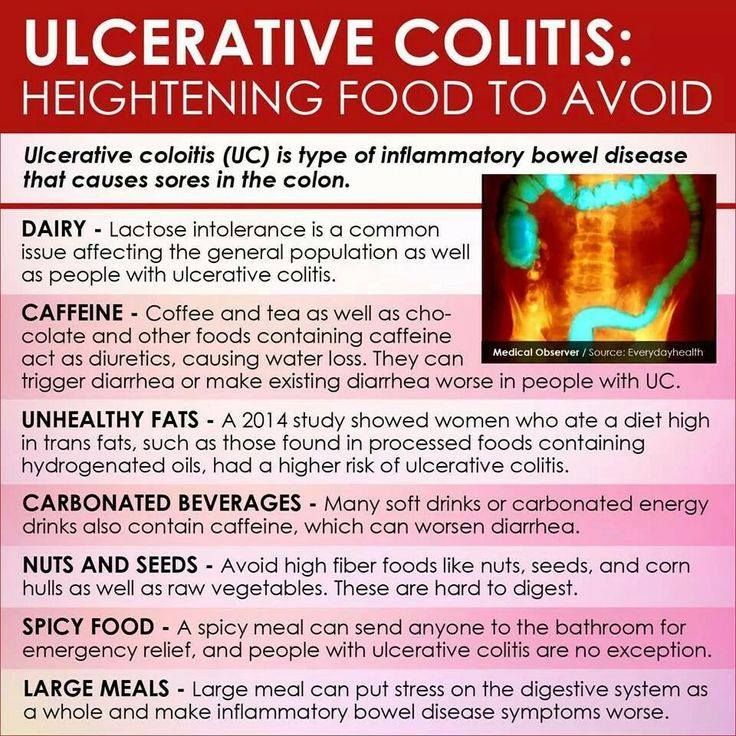
When youre in remission from ulcerative colitis, youll want to do everything you can to prevent a flareup. Things that may cause a flareup include:
- Emotional stress: Get at least seven hours of sleep a night, exercise regularly and find healthy ways to relieve stress, such as meditation.
- NSAID use: For pain relief or a fever, use acetaminophen instead of NSAIDs like Motrin® and Advil®.
- Antibiotics: Let your healthcare provider know if antibiotics trigger your symptoms.
Don’t Miss: Treating Leg Ulcers With Sugar
The Link Between Ulcerative Colitis And Stress
Stress can exacerbate colitis symptoms such as cramping and diarrhea. Heres how to find relief from uncomfortable flare-ups.
Stress does more than make your palms sweat and your brow furrow. For people with ulcerative colitis , it may bring on a painful flare.
Stress is well known for exacerbating inflammatory bowel disease symptoms, says Jordan Axelrad, MD, MPH, an assistant professor of medicine at NYUs Grossman School of Medicine and a gastroenterologist at NYU Langone Healths Inflammatory Bowel Disease Center in New York City. My patients always tell me that their symptoms feel worse when theyre stressed.
Causes And Risk Factors Of Ulcerative Colitis
Similar to several other diseases, health experts are not sure about the right causes of ulcerative colitis. A lot of health experts around the world believe that diet and a stressful lifestyle are one of the biggest causes of ulcerative colitis, but it is also not true.
The exact causes of ulcerative colitis are still unknown.
Some health experts around the world believe that immune system malfunction is also one of the biggest causes of ulcerative colitis. We already know that the immune system is known to fight itself if it is not working right, and it can also be the cause of ulcerative colitis.
At the same time, people with a family history of ulcerative colitis are more vulnerable to developing it in the future.
- Even though health experts believe that ulcerative colitis can occur at any age, it usually develops before the age of 30 or after the age of 60. We dont know the right causes, but the data has been suggesting the trend.
- At the same time, white people are also more vulnerable to developing the disease as compared to any other race. Health experts believe that Ashkenazi Jews are right and are in the highest risk category as compared to any other race.
- If you have a family history of ulcerative colitis, then health experts will suggest you consult with your healthcare provider anytime you visit for an annual checkup.
You May Like: How Ulcerative Colitis Is Diagnosed
How Stress Messes With Your Immune Response
If you are living with UC, stress talk gets elevated to a whole new level. Thats because UC is an inflammatory bowel disease that already causes inflammation in your digestive tract. So when you are experiencing stress, it can trigger even more inflammation in your body, leading to a worsening of UC symptoms. Stress affects UC as it would any chronic illness, says Loren Brook, M.D., a gastroenterologist at the University of Cincinnati College of Medicine in Ohio. Stress may increase your chances of flares and is known to weaken the immune system.
When you are stressed, the increase in cortisol can increase the pro-inflammatory cytokines and therefore cause increases in inflammation of the gut which has a negative effect on UC, says Bottoms. This also means your general immune system is not as effective and may struggle to fight against other illnesses as well.
Is Colitis In Dogs Deadly
Colitis is also very treatable and preventable.
Find out more here about what causes Colitis and how to make sure that your dog doesnât get it.
Colitis in dogs is an irritation of the colon and is a common malady.
The big ones are stress, infection or parasites, allergies, or any of several bowel diseases.
Don’t Miss: Do Ulcers Give You Diarrhea
How Is Ulcerative Colitis Treated
Theres no cure for ulcerative colitis, but treatments can calm the inflammation, help you feel better and get you back to your daily activities. Treatment also depends on the severity and the individual, so treatment depends on each persons needs. Usually, healthcare providers manage the disease with medications. If your tests reveal infections that are causing problems, your healthcare provider will treat those underlying conditions and see if that helps.
The goal of medication is to induce and maintain remission, and to improve the quality of life for people with ulcerative colitis. Healthcare providers use several types of medications to calm inflammation in your large intestine. Reducing the swelling and irritation lets the tissue heal. It can also relieve your symptoms so you have less pain and less diarrhea. For children, teenagers and adults, your provider may recommend:
Children and young teenagers are prescribed the same medications. In addition to medications, some doctors also recommend that children take vitamins to get the nutrients they need for health and growth that they may not have gotten through food due to the effects of the disease on the bowel. Ask your healthcare provider for specific advice about the need for vitamin supplementation for your child.
You might need surgery that removes your colon and rectum to:
- Avoid medication side effects.
- Prevent or treat colon cancer .
- Eliminate life-threatening complications such as bleeding.
Acute Psychological Stress And Gastrointestinal Motility And Water And Ion Secretion
Figure 2
Pathways by which the enteric nervous system is likely to mediate stress induced increases in inflammatory bowel disease symptomatolgy and disease activity. CRF, corticotrophin releasing factor SP, substance P IL, interleukin.
Acute psychological stress has effects on gastrointestinal motility, and water and ion secretion. Thus in healthy human volunteers, acute short term stress in the form of painful stimuli, dichotomous listening tests, and stressful interviews enhanced colonic motility. Dichotomous listening tests and cold pain stress have also been shown to increase jejunal water and sodium and chloride ion secretion. Although these are non-inflammatory changes, they could contribute to stress induced increases in symptomatology in patients with IBD.
You May Like: Medicines Used To Treat Ulcerative Colitis
Recommended Reading: Best Diet For Gerd And Ulcers
Painful And Strenuous Defecation
With colitis, dogs will strain while passing stool. This will cause pain. These are usually displayed when the dog squats to defecate. It will do so with a sense of urgency and display signs of discomfort and pain, unlike times when it is okay.
Flatulence, pronounced squatting and hunching, weight loss and disinterest in food are additional symptoms.
Ulcerative colitis can make life hard to predict. A flare-up of symptoms is stressful and can leave you worn out for days, weeks, or even months. Even in remission, you might get tired a lot or have a hard time meeting friends or going to work. Itâs easy to see why living with this long-term inflammatory disease can affect your mental health.
Theres no evidence that stress actually causes inflammatory bowel disease , which includes UC and Crohnâs disease. But stress can definitely bring on a flare-up. And youre more likely to feel anxious and depressed than your friends without UC. Your chances are even higher if you are a woman. Even rats with IBD in lab studies show signs of mood problems.
But there are steps you can take to lift your mood, even when your symptoms get you down.
What Is The Best Diet For Ulcerative Colitis
Theres no single diet that works best for ulcerative colitis. If the disease damages the lining of the colon, your body might not absorb enough nutrients from food. Your healthcare provider may recommend supplemental nutrition or vitamins. Its best to work with your provider and nutritionist to come up with a personalized diet plan.
Also Check: Stress And Ulcerative Colitis Flares
When Do You Consult A Doctor For Ulcerative Colitis
Once you have learned the basics about alternatives, once you have learned the basics about alternative quotes as common now, it is time for you to learn about the time when you should be consulting with your healthcare provider.
Even though we highly recommend everyone to go for an annual body checkup, as it is more capable of detecting diseases like ulcerative colitis, you can also consider the below-given points when it comes to consulting with your healthcare provider.
- If you are experiencing blood in your stool, you should call your healthcare provider right away. A lot of people think that blood in stool is usually caused by hemorrhoids, but it is not true.
- You are also supposed to consult with your healthcare provider if your abdominal pain is not going away.
- If you are experiencing diarrhea and it is not getting better even after taking medicine, you should consult with your healthcare provider.
These are the two conditions when you should not ignore the symptoms and consult with your healthcare provider as early as possible. A lot of people do not take these symptoms very seriously, but they can impose a huge risk, as the disease is known to cause life-threatening conditions.
What Can I Expect If I Have A Diagnosis Of Ulcerative Colitis
Ulcerative colitis is a lifelong condition that can have mild to severe symptoms. For most people, the symptoms come and go. Some people have just one episode and recover. A few others develop a nonstop form that rapidly advances. In up to 30% of people, the disease spreads from the rectum to the colon. When both the rectum and colon are affected, ulcerative symptoms can be worse and happen more often.
You may be able to manage the disease with medications. But surgery to remove your colon and rectum is the only cure. About 30% of people with ulcerative colitis need surgery.
Also Check: What Foods To Eat For Ulcerative Colitis
Ulcerative Colitis: Causes And Risk Factors
Causes
Experts dont know what causes ulcerative colitis, but it may be related to your immune system. Normally, your immune system attacks bacteria and viruses that could make you sick. However, with UC, the immune system mistakes the cells of your large intestine for a threat and attacks. When your immune system attacks your own healthy cells, it is referred to as an autoimmune condition. This causes inflammation and ulcers.
Why some people develop ulcerative colitis and not others is still being studied. It may have to do with genetic factors. You are more likely to develop UC if a family member has it. However, most cases develop in people without a family history.
Environmental factors, like exposure to certain viruses or bacteria, may also play a role. Your body may try to fight this infection and then overreact.
Doctors used to think that excess stress and certain foods cause ulcerative colitis, but we now know this isnt true. Diet and stress can make symptoms worse, but they dont cause them.
Risk factors
A risk factor is anything that increases your chance of developing a certain disease. Some risk factors for ulcerative colitis include:
Stress And Ulcerative Colitis
Experts havenât found an exact link. But they have some theories about the connection between the two.
Inflammation. Your body goes into fight-or-flight mode when stressed. That triggers the release of lots of chemicals, including cytokines. Those are molecules that turn on your immune system and lead to inflammation. People with UC might be more sensitive to this process.
Brain-gut axis. Stress changes the signals that travel between your brain and gut. This can cause all kinds of digestion problems, even in people who donât have UC. These changes are also linked to irritable bowel syndrome , food allergies, and heartburn.
Other reasons. Research shows stress might:
- Damage the lining of your gut
- Disturb gut bacteria
You can also just take a little time each day to do something you find relaxing. That could be gardening, reading, or listening to music. Whatever you enjoy.
Drug therapy is another option. Studies show antidepressants might ease pain in people with IBD. Common choices include selective serotonin reuptake inhibitors and tricyclic antidepressants . Ask your doctor if theyâre right for you.
Read Also: Can Ulcerative Colitis Cause Constipation
Psychological Stress And Gastrointestinal Motility And Water And Ion Secretion
As in humans, acute stress in the form of restraint stress, loud noise, inescapable foot shock, or water avoidance all increase colonic motility and defecation in the rodent. The mechanisms for these changes involve CRF and its receptors .
Similar alterations in ion and water transport to those seen in humans are also well described in animals in response to psychological stress. Increases in gastrointestinal water and chloride ion secretion occur in response to restraint stress in the rat. It is now recognised that, as with changes in intestinal permeability, this secretory response is related to both cholinergic nerves and mast cells as it was increased in cholinesterase deficient Wistar-Kyoto rats, blocked by pretreatment with atropine, and absent in mast cell deficient rats. Restraint stress also increased colonic mucus secretion in ex vivo colonic segments and in vivo, as measured by histological goblet cell depletion. This effect could also be reproduced by peripheral CRF administration and inhibited by mast cell stabilisers.
What Should I Ask My Doctor On Behalf Of My Child Or Teenager
Ask your healthcare provider the following questions in addition to the ones listed above:
- What vitamins should my child take?
- Will my other children have pediatric ulcerative colitis?
- Is my child at risk for other conditions?
- Can you recommend a psychiatrist or therapist to help my child with emotional issues related to pediatric ulcerative colitis?
- Is my child growing at a normal rate?
- What can I do to help my child cope at school?
A note from Cleveland Clinic
When you have ulcerative colitis, its essential to work closely with your healthcare team.
Take your medications as prescribed, even when you dont have symptoms. Skipping medications youre supposed to take can lead to flareups and make the disease harder to control. Your best shot at managing ulcerative colitis is to follow your treatment plan and talk to your healthcare provider regularly.
You May Like: What Vegetables Are Good For Ulcerative Colitis
Understanding Stress And Anxiety In Ibd
Video Length1:25
Understanding Stress and Anxiety in IBD While stress and anxiety has not been shown to cause Crohn’s disease or ulcerative colitis, they can certainly have an impact on your disease. Learn more!
- Transcript
|
|
|
|
|