Medical History And Examination
Your GP or practice nurse will ask whether you have any other symptoms associated with venous leg ulcers, such as:
- swelling in your ankles
- discoloured or hard skin
They’ll try to determine the cause of the ulcer by asking about underlying conditions or previous injuries, such as:
Read more about how venous leg ulcers are treated.
Deterrence And Patient Education
Individuals affected with VLUs can have an impaired quality of life, mainly related to disability. Plus, heavy exudates can cause malodor, social isolation, and emotional disturbances that severely impact life quality. Compliance is essential to achieve a successful outcome.
Patients should be educated because VLUs are chronic processes that require lifelong evaluation and care, even after wound closure. Additionally, conformity to diet and lifestyle modifications may reduce the risk or recurrence, but evidence is lacking.
What Types Of Venous Disease Cause Venous Stasis Ulcers
Chronic venous insufficiency is a common cause of valve dysfunction. It occurs when your valves are damaged or too weak to do their job.
Other venous ulcer causes include:
- High blood pressure , which damages blood vessel walls.
- Venous obstruction, a vein blockage thats sometimes due to blood clots.
- Venous reflux, when blood flows backward through weak or damaged valves.
You May Like: Compression Therapy For Venous Leg Ulcers
Signs Of An Infection
A venous leg ulcer can be susceptible to bacterial infection. Symptoms of an infected leg ulcer can include:
- worsening pain
A number of factors can increase your risk of developing a venous leg ulcer, including:
- obesity or being overweight this increases the pressure in the leg veins
- if you have difficulty walking this can weaken the calf muscles, which can affect circulation in the leg veins
- previous deep vein thrombosis blood clots that develop in the leg can damage valves in the veins
- varicose veins swollen and enlarged veins caused by malfunctioning valves
- previous injury to the leg, such as a broken or fractured bone, which may cause DVT or impair walking
- previous surgery to the leg, such as a hip replacement or knee replacement, which can prevent you from moving about
- increasing age people find it harder to move around as they get older, particularly if they suffer from arthritis
Symptoms Of Venous Insufficiency Ulcers
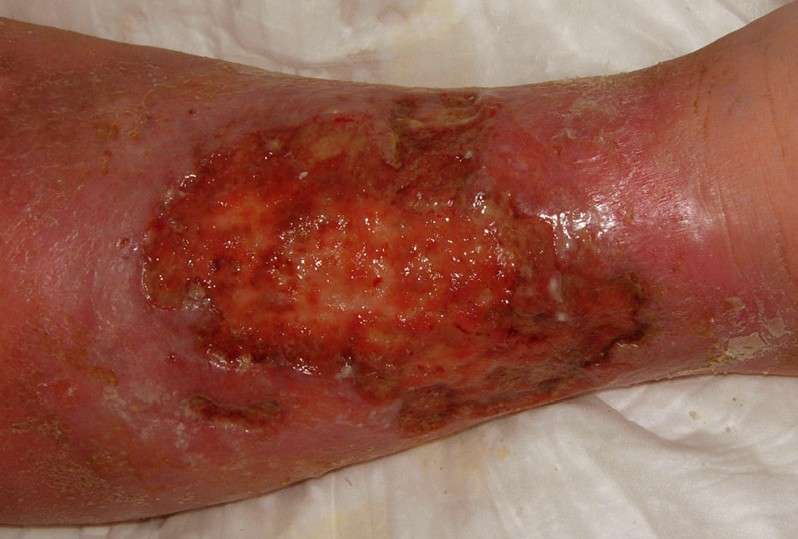
Whe a venous ulcer begins to develop, stasis dermatitis may be present causing scaling and erythema of the lower extremities. Hemosiderin staining may also occur, causing the presence of brownish or yellow patches underneath the skin. Other skin changes may include the appearance of dark red or purple as a result of blood leaching into the surrounding tissue. Venous ulcers will present with shallow but large wounds with irregular margins that typically develop on the lower leg or ankle. The base of the ulcer is typically red, can result in a significant amount of exudate depending on the level of infection, and will ooze venous blood when manipulated. Typically the wound will be relatively painless, with any pain resulting from subsequent infection or edema. Often the entire leg will become swollen, and the skin will become more firm and reddish brown in color, otherwise known as stasis dermatitis. Elevation of the limb will help to relieve discomfort and swelling.
Figure 1: Venous ulcer with obesity as cofactorFigure 2: Large superficial venous ulcer
Also Check: Interprofessional Care For Ulcerative Colitis
Cleaning And Dressing The Ulcer
The first step is to remove any debris or dead tissue from the ulcer and apply an appropriate dressing. This provides the best conditions for the ulcer to heal.
A simple non-sticky dressing will be used to dress your ulcer. This usually needs to be changed once a week.
Many people find they can manage cleaning and dressing their own ulcer under the supervision of a nurse.
What Causes Vascular Ulcers
Vascular ulcers can typically be grouped by their cause. However, it’s common for multiple conditions to cause an ulcer. An example of this is how diabetes can cause vascular ulcers.
- Stasis ulcers. Caused by vein problems, these make up the majority of vascular ulcers. These are most common in your legs and feet as you age and happen because the valves in your leg veins cant do their job properly. This means they cant stop blood which should be headed upward to your heart from being pulled down by gravity. As a result, the excess blood in your legs and feet puts too much pressure on the blood vessels, which leak and burst. Over time, this can ulcers to develop.
- Arterial ulcers. These are also called ischemic ulcers. These happen because of limited blood flow to an affected area, a problem called ischemia . The affected body part, usually a limb, slowly dies because of a lack of blood flow.
Read Also: What Causes H Pylori Ulcers
Treatment Options For Venous Stasis Ulcers
At first, venous ulcers are generally shallow and irregularly shaped. As the deterioration of the affected tissue progresses, the ulcer can extend deeper into the underlying tissues, involving the tendons, ligaments, and bone. The goal of venous ulcer treatment is to minimize edema, control infection, heal the wound, and prevent reoccurrence. Many leg ulcer patients experience alternating periods of healed and open ulcerations. Those with venous stasis ulcer commonly find the skin lesions will return unless the underlying cause is corrected.
To effectively treat venous stasis ulcers, doctors commonly evaluate the venous and arterial circulation in the affected area to identify the underlying cause. Once the cause is determined, physicians are in a better position to develop a successful plan of action. Doctors treating venous ulcers may recommend one or more of the following options:
What Are Venous Stasis Ulcers
Commonly located on the ankle or calf, venous stasis ulcers are painful and red in color but may be covered with a yellow, fibrous tissue and an irregular border.
Drainage and discharge are possible with venous stasis ulcers. This type of ulcer is common in patients with a history of leg swelling or varicose veins.
Read Also: Can Ulcerative Colitis Cause Blood In Urine
What Is The Treatment For Venous Stasis
4.4/5treatment for venous insufficiency
Likewise, people ask, does venous stasis go away?
These venous stasis ulcers can be difficult to heal and can become infected. When the infection is not controlled, it can spread to surrounding tissue, a condition known as cellulitis. CVI is often associated with varicose veins, which are twisted, enlarged veins close to the surface of the skin.
Likewise, can exercise help venous insufficiency? Treatment for chronic venous insufficiencyExercise: Exercise helps pump blood through the legs and builds muscle that can promote better circulation. A doctor may also instruct a patient to elevate the legs above the heart three or four time a day for about 15 minutes at a time. This can help to reduce swelling.
Considering this, is walking good for venous insufficiency?
Your doctor may recommend that you walk, ride a stationary bicycle, or jog for 30 minutes several times a week. Being active helps improve circulation and tones muscles in your legs. This can help pump blood toward the heart. Stretching your calf and thigh muscles can also help improve blood flow.
Is venous insufficiency serious?
Vein disease is incredibly common â and manageable. However, if left untreated, venous insufficiency can cause far more serious complications like ulcers, bleeding, and a life-threatening condition called deep vein thrombosis .
Skin Grafts And Artificial Skin
Two layers of skin created from animal sources as a skin graft has been found to be useful in venous leg ulcers.
Artificial skin, made of collagen and cultured skin cells, is also used to cover venous ulcers and excrete growth factors to help them heal. A systematic review found that bilayer artificial skin with compression bandaging is useful in the healing of venous ulcers when compared to simple dressings.
You May Like: Cbd Oil For Stomach Ulcers
Who Gets Foot And Toe Ulcers
Youre at higher risk for foot and toe ulcers if you are:
- Native American.
- Male.
- Elderly.
If you have an eye, kidney or heart disease related to diabetes, youre also at a higher risk. About 15% of people with diabetes will get an ulcer, typically on the bottom of their foot. Around 6% of that 15% will have to be hospitalized because of complications.
Youre also at a higher risk of getting foot and toe ulcers if you have any of the following:
- Problems with circulation.
Common Causes Of Stasis Dermatitis
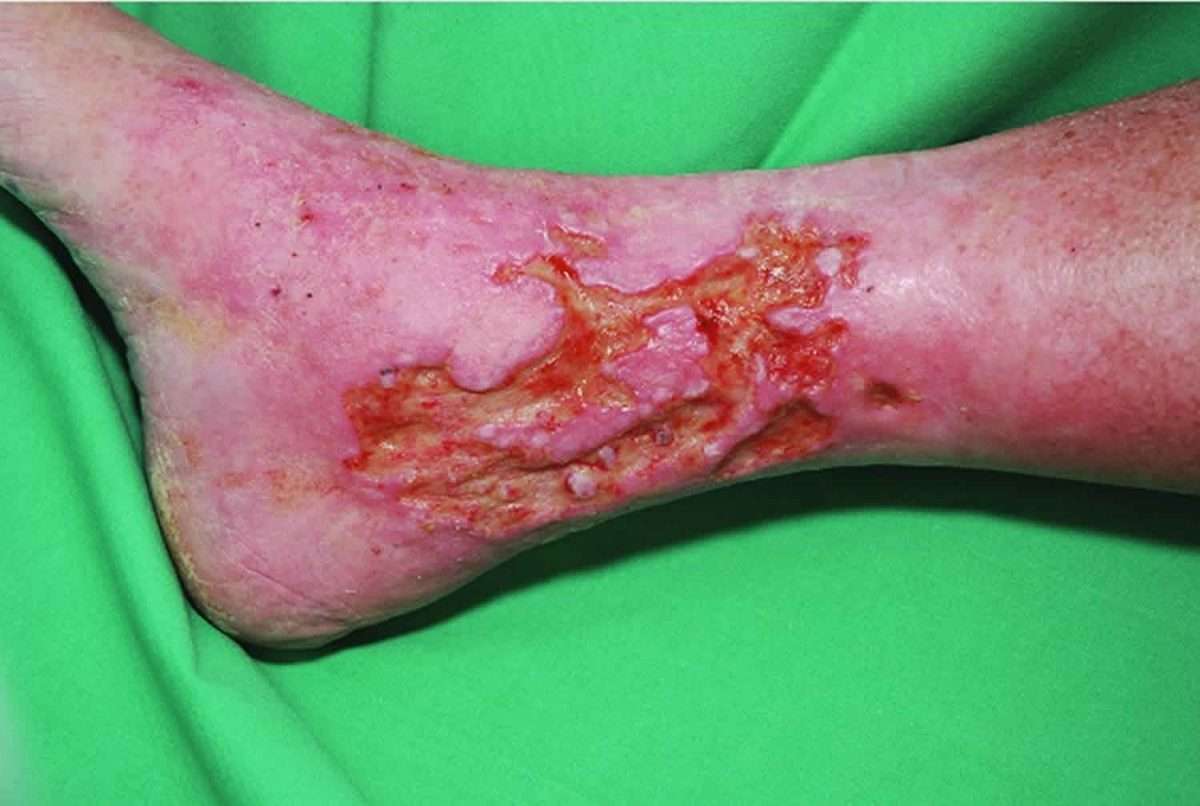
Poor circulation causes stasis dermatitis. Typically, poor circulation is the result of a chronic condition called venous insufficiency. Venous insufficiency occurs when your veins have trouble sending blood to your heart.
There are one-way valves inside your leg veins that keep your blood flowing in the right direction, which is toward your heart. In people with venous insufficiency, these valves become weak. This allows blood to flow back toward the feet and pool in your legs instead of continuing to flow toward your heart. This pooling of blood is what causes stasis dermatitis.
Varicose veins and congestive heart failure are also known causes of leg swelling and stasis dermatitis.
Most of the conditions that cause stasis dermatitis usually develop in people as they get older. However, there are also several causes that are unrelated to age, including:
- surgery, such as using a leg vein for bypass surgery
Ask your doctor about the types of skin creams and ointments you can use. Avoid using the following products:
- lanolin
- calamine and other lotions that dry your skin
- topical antibiotic ointments such a neomycin, due to possible allergic reactions
- benzocaine and other numbing medications
Your doctor might tell you to put wet bandages on your skin and might prescribe topical steroid creams and ointments. Your doctor may also prescribe antibiotics if your skin becomes infected. Surgery may be recommended to correct varicose veins if they become painful.
- chronic leg ulcers
Read Also: Hydrocolloid Dressing For Stage 1 Pressure Ulcer
Making Healthy Lifestyle Choices
Maintaining a healthy lifestyle has a direct impact on vein health. A nutritious diet, regular exercise, maintaining a healthy weight, and following the recommendations of your health care provider can slow the progression of vein disease, ensure the successful outcome of vein treatment, and promote healing.
How Do You Describe A Venous Stasis Ulcer
Venous stasisveinsVenous ulcers
. Keeping this in consideration, what does venous stasis ulcer look like?
Symptoms of Venous Insufficiency UlcersVenous ulcers will present with shallow but large wounds with irregular margins that typically develop on the lower leg or ankle. Often the entire leg will become swollen, and the skin will become more firm and reddish brown in color, otherwise known as stasis dermatitis.
Likewise, how long does it take a venous stasis ulcer to heal? 12 weeks
Thereof, how do you describe a venous ulcer?
Signs and symptoms of venous ulcers include:
Don’t Miss: Does Ulcerative Colitis Cause Back Pain
How Do You Know When A Leg Ulcer Is Healing
These wounds should be showing signs of healing within 2 weeks of injury. If a wound is taking longer than a couple of weeks to show signs of healing or the wound is weeping and getting larger, then this might be a sign of an underlying problem which needs looking into.
Do leg ulcers ever heal?
Most venous leg ulcers heal within 3 to 4 months if theyre treated by a healthcare professional trained in compression therapy for leg ulcers. But some ulcers may take longer to heal, and a very small number never heal. Treatment usually involves: cleaning and dressing the wound.
Dont Miss: Ulcers On Legs From Diabetes
Referral To A Specialist
In some cases, your GP or nurse may decide to refer you to a specialist in conditions affecting the blood vessels .
For example, you may be referred to a vascular specialist if your GP or nurse is unsure about your diagnosis, or if they suspect your ulcer may be caused by artery diseases, diabetes or rheumatoid arthritis.
After taking your medical history and examining you, the vascular specialist may need to arrange further investigations to plan your treatment.
Recommended Reading: What Does A Colon Ulcer Feel Like
What Is A Vascular Ulcer
Vascular ulcers are wounds on your skin that develop because of problems with blood circulation. They are most common on your limbs especially your lower legs and feet but can also develop elsewhere on your body. These wounds can take a very long time to heal and may need specialized treatment, including surgery.
Vascular ulcers can have two different causes. One is from poor circulation in your arteries, which provide nutrients and oxygen to the body. The other type of vascular ulcer is caused by poor circulation in your veins, which takes blood and waste products from the body and returns them to the heart. The most common type of vascular ulcer is a venous ulcer.
How common are vascular ulcers?
Vascular ulcers are very common, especially as people age. About 1% of adults in the U.S. have a vascular ulcer. For adults over the age of 65, it can be between 3% and 5%.
Venous Ulcer Diagnosis And Treatment
Doctors at Vascular surgeons at UPMC’s Heart and Vascular Institute use duplex ultrasound, a noninvasive test, to diagnose abnormal veins that cause venous ulcers. Part of the UPMC difference is that we actively look for the causes of the ulceration to treat venous pathology and keep the ulcer healed.
After an evaluation of your veins, we recommend a treatment plan based on your needs:
- Compression
- Compression of the leg is vital to healing venous wounds.
- Compression stockings are most commonly used for this treatment.
- The pressure from the compression dressing counteracts the pressure from the veins of the leg and allows skin to heal.
Don’t Miss: How To Prevent Sacral Pressure Ulcers
Other Types Of Leg Ulcer
Other common types of leg ulcer include:
- arterial leg ulcers caused by poor blood circulation in the arteries
- diabetic leg ulcers caused by the high blood sugar associated with diabetes
- vasculitic leg ulcers associated with chronic inflammatory disorders such as rheumatoid arthritis and lupus
- traumatic leg ulcers caused by injury to the leg
- malignant leg ulcers caused by a tumour of the skin of the leg
Most ulcers caused by artery disease or diabetes occur on the foot rather than the leg.
Page last reviewed: 11 January 2019 Next review due: 11 January 2022
Venous Stasis Ulcer Symptoms
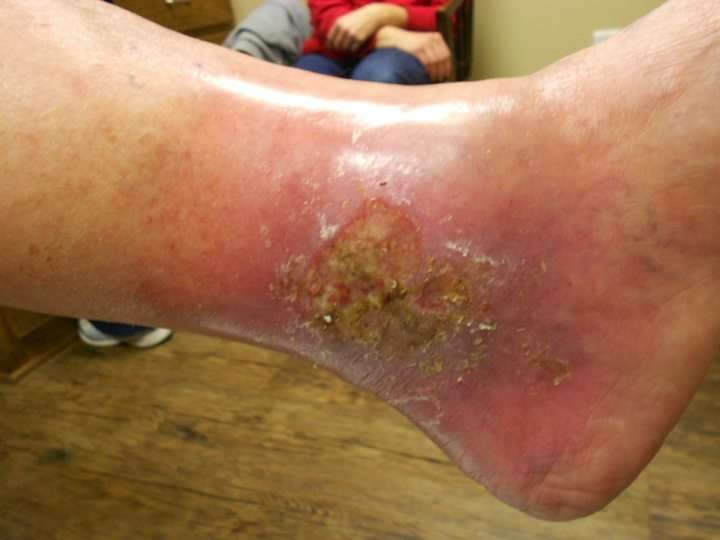
The development of an venous stasis ulcer is a serious medical condition that is usually preceded by a series of symptoms, including:
- The development of stasis dermatitis, a condition usually observed in the lower legs and characterized by itchy skin, fluid retention, and noticeable changes in skin color and texture.
- Swelling
- A general heaviness in the limbs of the affected area.
The venous stasis ulcer itself has several distinct characteristics, including:
- Being a shallow sore with a red or purple base accompanied by the appearance of yellow, crust-like tissue around the perimeter of the sore
- A brownish discoloration of the skin surrounding the venous stasis ulcer
- The affected area being warm/hot to the touch
- Localized pain
- Oozing of pus
Unlike most wounds of the skin, which tend to heal quickly, a venous stasis ulcer lacks the proper oxygen and nutrients required to support the natural healing process this often results in prolonged or poor healing and a significant increase in the risk of infection.
Read Also: How Can I Ease The Pain Of A Stomach Ulcer
What Is Venous Stasis
Venous stasis is the swirling, slowing down or pooling of blood inside leg veins. This condition is also called venostasis. This pooling is a direct result of malfunctioning vein valves, sitting for too long or varicose veins. When malfunctioning vein valves are left untreated, and as it progresses, venous stasis can cause increasing pain and swelling in affected areas while also increasing the risk of blood clots and contributing to the formation of varicose veins, venous stasis ulcers, and stasis dermatitis.
Most often observed in the legs, this condition is more common in people with chronic venous insufficiency and people who travel often.
Venous Insufficiency And Venous Ulcers
Venous insufficiency, also called venous reflux, is a debilitating leg issue in which the blood cant flow up through the veins toward the heart. Healthy veins contain a number of specialized, one-way valves that open to allow blood to flow upward and close to prevent blood from flowing back down. When these valves are damaged or malfunctioning, venous insufficiency occurs.
As the valves deteriorate, the blood flows backwards and increases the pressure in the vein, dilating it. Blood stagnates, or pools, in the veins of the lower legs, putting pressure on the venous wall and causing inflammation and discomfort.
In many patients, untreated superficial venous reflux leads to the deposition of red blood cells in the tissues. Hemoglobin, the protein in red blood cells that carries oxygen, and hemosiderin, the accumulation of iron from the breakdown of hemoglobin , leaves deposits in the skin in the form of dark staining.
In severe cases, chronic, untreated venous insufficiency can cause open sores to develop on the skin, known as venous ulcers. These ulcers occur at the site where blood pools, due to the swelling that prevents the movement of nutrients and oxygen to the tissues.
Venous insufficiency can also cause varicose veins, a condition in which the superficial veins, or the veins closest to the surface of the leg, enlarge, twist, or bulge. In addition to being unsightly, varicose veins can cause pain, discomfort, or the development of venous ulcers.
Also Check: Icd 10 Venous Stasis Ulcer Left Leg